
Boiling Point
OSHA Must Act Immediately to Protect Workers From Deadly Temperatures
By Juley Fulcher
Key Findings
Fifty years ago, the National Institute for Occupational Safety and Health (NIOSH) called for rules to protect workers from unsafe heat. Five decades later, the Occupational Safety and Health Administration (OSHA) has still failed to put such rules in place, although it finally began work on creating a standard in 2021.
With the climate crisis shattering heat records each summer, heat stress is a rapidly worsening threat for workers across the country, demanding immediate action.
- Environmental heat is likely responsible for 170,000 work-related injuries every year, and possibly many more. If documented accurately, environmental heat would rank as high as third among causes of occupational injuries and illnesses.
- Heat exposure is responsible for 600-to-2,000 worker fatalities, annually, ranking it among the top three causes – and possibly the top cause – of occupational fatalities.
- Farm workers – the vast majority of whom are immigrants, many undocumented – are the most vulnerable to heat-related injury and death.
- Worker heat-stress tragedies disproportionately strike workers who are poor, Black or Brown.
- The central elements of a heat protective workplace standard are very simple: providing adequate water, shade and breaks.
- A heat-safety standard issued by California reduced injuries by 30%. This suggests that at least 50,000 injuries and illnesses could be avoided nationwide if OSHA adopted a simple heat standard.
In light of the severity of the environmental heat crisis and the known efficacy of protective measures, OSHA should issue an Emergency Temporary Standard while it continues the slow process of proposing and finalizing a permanent standard.
Executive Summary
Extreme heat is endangering the lives and well-being of workers – disproportionately Hispanic/Latino or African-American – who work under the midday sun or in stifling indoor conditions. The National Institute for Occupational Safety and Health identified heat stress as significant workplace hazard 50 years ago; the problem is growing far more severe due to the ravages of the climate crisis.
The Occupational Safety and Health Administration is required by law to ensure that American workers are provided with “safe and healthful” conditions. In 2011, Public Citizen and others petitioned OSHA to issue a long overdue rule to protect workers from environmental heat. The agency denied the petition. Public Citizen and allies petitioned again in 2018 for a permanent rule, and for an emergency temporary standard in 2021. In 2021, OSHA announced it was starting the process to issue a permanent rule, but that process is anticipated to take six-to-eight years.
Estimates contained in this report place heat among the highest-ranking causes of injuries and fatalities for American workers.
Taking action will protect workers. A heat-safety standard in California resulted in a 30% reduction in heat-related injuries and illnesses. These results suggest that a national standard would prevent more than 50,000 heat-related injuries and illnesses a year.
Abundant research indicates that the sorts of protections that workers need to function safely are not complicated. Items such as access to water and periodic rest breaks in a cool location top the list.
Such commonsense steps might seem so obvious that no standard is necessary. But until OSHA requires them in a legally binding rule, employers’ implementation of them will be inconsistent – and tens of thousands of workers will continue to suffer senseless injuries and deaths.
I. Rising Temperature Are Demolishing Previous Records
Changes to the Earth’s climate ordinarily occur in tiny increments over hundreds, thousands or, even, millions, of years. But marked changes to temperatures are seemingly occurring before our eyes.
Globally, average temperatures for each of the past 45 consecutive years have exceeded average temperatures for the 20th century. The nine years spanning 2013 to 2021 were all among the 10 hottest years since record keeping began in 1880.[1] The National Oceanic and Atmospheric Administration says there is a greater than 99% chance that 2022 will be among the 10 hottest years on record.[2]
June 2021 was the hottest June ever recorded in the United States,[3] as was the entire summer of 2021.[4] July 2021 was the hottest month ever recorded on Earth.[5] In addition to the 1,238 daytime heat records set in June of 2021 in the U.S, more than 1,500 nighttime heat records were broken.[6] Notably, a heat wave is defined by the how much it cools down at night.[7]
Canada experienced new all-time high temperature records for three consecutive days in June 2021, peaking at 121 degrees in a British Columbia village. Portland, Ore., and Seattle also experienced all-time highs in this period. Portland’s 115 degree reading was nine degrees higher than the previous record.[8]
These conditions are dangerous for anyone who is not protected from the elements. Approximately 1,200 people are believed to have died in the June 2021 Pacific Northwest heat wave.[9]
Extreme heat waves, like the one that occurred in the Pacific Northwest in June 2021, now occur five times more often than they did prior to 1900.[10]
Climate change has also resulted in devastating storms, droughts and wildfires. Eight of California’s 10 largest wildfires have occurred in the last five years.[11] Two of those wildfires burned areas larger than Rhode Island.[12]
The dangers of extreme heat are greatest for people who are poor, elderly and/or forced to labor in unsafe temperatures for their livelihood. Those at risk, including the workers, are disproportionately people of color.
II. Soaring Temperatures Have Created a Crisis for Workers
The human body has a complex regulatory system designed to keep our core temperature about 98.6 degrees. Heat stress refers to strain on that system as it tries to keep the body cool. The heat comes from both external environmental conditions and the heat generated inside our bodies, or metabolic heat.[13]
The amount of physical effort needed for peoples’ workloads increases their metabolic heat production. The ambient temperature and radiant heat sources like direct sunlight and heat-generating machinery add to heat stress.[14]
An important strategy for the body to dissipate heat is to use evaporative cooling through sweat. Another mechanism is to increase blood flow to the skin, where it can be cooled by releasing body heat into the cooler surrounding environment.[15]
Environmental conditions can hamper the regulatory system’s ability to keep the body cool. As temperatures rise, heat exchange acts in the opposite direction. Instead of heat being released from the body when blood flows to the skin, more heat is introduced into the body. That leaves only evaporative cooling as a mechanism to regulate temperature.
High humidity limits evaporation of sweat. For this reason, ambient temperature may not effectively convey the heat stress danger. It’s more useful to rely on the heat index, or apparent temperature, which combines ambient temperature and relative humidity to describe what it feels like to our bodies. Heat, humidity and other modifying factors can have a dramatic impact on the health and safety of workers, whether indoors or outdoors.
As the body struggles with excessive heat stress, we experience heat strain.[16] When a worker is pushed beyond a safe heat exposure for the workload, a range of dangerous illnesses may result:
Heat exhaustion — Working in high temperatures can lead to headaches, nausea, dizziness, weakness, irritability, thirst, and elevated body temperature.[17] Heat exhaustion can contribute to workplace accidents.
Heat syncope — Dizziness, light-headedness, or fainting with prolonged standing or sudden rising within a hot environment puts workers at great risk of injury.[18]
Rhabdomyolsis — Prolonged physical exertion in hot weather, coupled with dehydration, can lead to muscle cramps and, in severe cases, a life-threatening rapid breakdown and death of muscle tissue that can lead to acute kidney injury.[19]
Acute Kidney Injury — High workloads and limited access to adequate hydration can cause a reduction in kidney function.[20]
Heat stroke — If heat exhaustion becomes severe, then heat stroke, a life-threatening medical emergency, can occur. During a heat stroke, the body rapidly loses the ability to regulate temperature and is no longer able to sweat. The body’s temperature can rise to 106 degrees or higher within 10 to 15 minutes, and if immediate medical attention is not secured, death can come quickly.[21]
A. Environmental Heat Is One of the Greatest Causes of Workplace Injuries and Deaths in the United States
Official data on workplace injuries and illnesses is disseminated by the Bureau of Labor Statistics (BLS), which bases its conclusions on surveys of employers. This data is notoriously unreliable because it relies on self-reporting, and less than half of employers even maintain the required records.[22]
Data estimating injuries and illnesses from heat is further hampered by the difficulty of deeming “exposure to environmental heat” (the relevant BLS category) to be the chief cause out of hundreds of category choices when an injury or illness potentially caused by heat occurs.
Further, despite the use of the term “injuries and illnesses” in the categorization of heat-related worker harms by both BLS and OSHA, the data only reflect heat illnesses, not the injuries that are caused by the effects of heat stress. OSHA’s guidance on record-keeping regarding adverse outcomes from heat only references illnesses caused by excessive heat “such as heat illness, heat stroke, kidney injury and rhabdomyolysis.”[23] In reality, heat may be a determinative factor in many injuries. For example, if an employee becomes dizzy from high temperatures and falls off a ladder, her injury would be reported to the BLS under the heading of “Falls, Slips, Trips.” As the contents of this report show, higher temperatures are correlated with greater numbers of injuries.
For what it’s worth, which is not much, the BLS data indicate that there were about 3,400 workplace heat-related injuries and illnesses requiring days away from work per year from 2011 to 2020.[24] Over the same 10 years, BLS estimates show an average of 40 heat-related fatalities per year in the workplace.[25]
OSHA acknowledges, “the estimates provided [by BLS] on occupational heat-related illnesses, injuries, and fatalities are likely vast underestimates.”[26]
1) Extrapolations of Data From California Workers’ Compensation Claims Suggests That Heat Is Among the Top Causes of Workplace Injuries and Illnesses in the U.S.
An analysis of more than 11 million workers’ compensation injury reports in California from 2001 through 2018 found that working on days with hotter temperatures likely caused about 20,000 injuries and illnesses per year in that state, alone — an extraordinary 300 times the annual number injuries and illnesses that California OSHA (Cal/OSHA) attributes to heat.[27]
The results of the California study are instructive in estimating the extent of uncounted heat-related injuries nationwide. If California’s workers suffer approximately 20,000 heat-related injuries and illnesses per year, a simple extrapolation based on the worker population of other states[28] suggests that the number suffered by all U.S. workers is likely in the range of 170,000 heat-related injuries and illnesses per year.[29]
That would make environmental heat one of the greatest causes of occupational injury and illness nationwide. Table 1, below, shows the top 10 causes of injuries and illnesses requiring days way from work by average per year since 2011. At 170,000 annual cases per year, environmental heat would rank third on this list.
Table 1: Average Number of Events or Exposures Causing Days Away From Work in the U.S., 2011-2020
| Event or Exposure† | Cases |
| 1. Overexertion involving outside sources | 240,998 |
| 2. Falls on same level | 185,724 |
| Exposure to environmental heat | 170,000* |
| 3. Struck by object or equipment | 151,116 |
| 4. Other exertions or bodily reactions | 85,119 |
| 5. Exposure to other harmful substances | 65,344^ |
| 6. Falls to lower level | 58,155 |
| 7. Struck against object or equipment | 57,993 |
| 8. Slip or trip without fall | 45,909 |
| 9. Roadway incidents involving motorized land vehicle | 43,031 |
| 10. Caught in or compressed by equipment or objects | 36,314 |
Source: Bureau of Labor Statistics and Public Citizen.
† BLS injury and illness records are broken into seven broad categories, which carry one digit codes. Under those categories are 46 discrete causes of injuries and illnesses, which carry two digit codes. More than 300 three-digit and four-digit subcategories fall under those. Table 1 lists the top causes of injuries and illnesses among the two-digit categories. The official BLS category “Exposure to environmental heat” is a three-digit category.
^ The 2020 BLS reported cases for this category were unusually high due to COVID cases. Recorded cases in 2020 were more than 20 times the average for the previous nine years.
* Estimate by Public Citizen using extrapolation from findings in an academic study on workplace injuries.
This estimate and methodology come with a caveat: Just as applying a more focused lens on estimates of injuries and illnesses from workplace heat results in a significantly higher estimate of annual cases, the same would likely be true for many other events and exposures. They are likely undercounted as well. What this exercise shows is not necessarily that environmental heat is the third-greatest cause of workplace injuries, but that it is a very significant cause, whatever its specific rank might be.
2) Heat Is Also Likely Among the Greatest Causes of Occupational Deaths in the U.S.
The BLS Census of Fatal Occupational Injuries indicates that 400 U.S. workers died from occupational heat stress between 2011 and 2020, an average of 40 per year.[30]
We know this number grossly underestimates actual heat-related occupational fatalities. Determination of the cause of death relies rely primarily on the conclusions recorded in death certificates and the judgment of medical professionals making those findings.[31] This information is notoriously problematic in the case of heat stress.[32]
The U.S. Centers for Disease Control and Prevention (CDC) estimates there are approximately 700 annual heat-related deaths among the general population, i.e., including fatalities occurring outside of work settings as well as on the job.[33] The estimates rely on data collected from death certificates that listed heat as the underlying or contributing cause of death.[34]
The U.S. Environmental Protection Agency also attempts to estimate heat-related fatalities. Its analysis, which covers a longer timeframe, arrives a similar but slightly lower estimate of about 600 heat-related fatalities per year. Importantly, the EPA has said, “It has been well documented that many deaths associated with extreme heat are not identified as such by the medical examiner and might not be properly coded on the death certificate.”[35] EPA notes that deaths from heart conditions and respiratory diseases with heat stress as a contributing factor are much more common than deaths from heat stroke and other heat-related illnesses.[36] But exposure to excessive heat often may not be identified as the underlying reason for the death.
Recent research is instructive in estimating the extent of the undercount of workplace heat-related deaths.
A compelling 2020 study (Weinberger et al.) cross-referenced a decade’s worth of fatality data by date and location with corresponding temperature data to arrive at an estimate of excess fatalities due to high temperatures. The study examined data in 297 U.S. counties across 44 states and the District of Columbia, encompassing 62% of the total U.S. population.[37]
The study estimated that 5,608 deaths per year in those jurisdictions were attributable to heat.[38] The diversity of climates in the studied counties makes it reasonable to expand the study’s findings to the entire U.S. population. This results in an estimate of 9,079 heat-related fatalities per year.[39] The study used data from 1997 to 2006. If it used more recent data, it would almost certainly have arrived at a higher estimate of heat-related deaths because temperatures in the United States have risen significantly in recent years.
Another study published in 2020 (Shindell et al.) compared temperature and mortality data from 2010 to 2019 in 10 cities across the United States. Incorporating location-specific climate data, the study identified the relative risk of premature fatalities associated with incremental changes in temperature for each city. Using the findings from the 10 cities, the study estimated 12,000 heat-related fatalities occur each year in the entire United States.[40]
The estimates of the Weinberger et al. and Shindell et al. studies do not provide direct insight into the number of workplace heat-related fatalities. But it would be possible to derive an estimate of the number of heat-related workplace fatalities from the studies if the ratio between heat-related workplace and total fatalities were known. One way to estimate this ratio is to divide the BLS-calculated workplace heat-related fatalities by the CDC-calculated total heat-related fatalities. The heat-related fatality estimates by these two government agencies are derived using similar methodologies using death certificates and, thus, offer a credible lens into the ratio of workplace heat-related fatalities to total such fatalities.
Here’s how the math works out. The BLS-calculated workplace heat-related fatalities per year is 40. The CDC-calculated total heat-related fatalities per year is 702. Boiling down the fraction of 40/700 yields 1/17th. This means that the government’s data suggests that one-in-seventeen heat-related fatalities is work related.
To apply the findings of Weinberger et al., we then take 1/17th of the estimated 9,076 annual heat-related fatalities suggested by their study. This yields an estimate that 605 occupational heat-related fatalities occur every year. Applying the same extrapolation to the Shindell et al. study, we take 1/17th of the estimated 12,000 heat-related fatalities posed by their study. This yields an estimate of 706 occupational heat-related fatalities every year. [Table 2]
Table 2: Estimated Annual Heat-Related Workplace Fatalities Derived by Applying Academic Estimates on Total Heat-related Fatalities to Federal Data on Work Vs. Total Heat-related Fatalities
| Study | Estimate of Total Heat-related Fatalities | Ratio of Workplace-to-Total Heat-related Fatalities in Government Data | Annual Workplace Heat-related Fatality Extrapolation |
| Weinberger et al. | 9,079 | 1:17 | 605 |
| Shindell et al. | 12,000 | 1:17 | 706 |
A separate but analogous way to use the Weinberger et al. and Shindell et al. studies in concert with other studies is to compare the number of heat-related injuries reported in the 2020 Park et al. study to the heat-related injuries reported by BLS. If the discrepancy in fatalities can fairly be assumed to match the discrepancy in injuries, the Park-to-BLS injury ratio could used to derive estimates on the number of fatalities.
Again, here’s the math. The Park et al. study concluded that there are about 20,000 annual heat-related injuries in California. This extrapolates to about 170,000 nationwide. The BLS reports an average of 3,400 annual heat-related illnesses and injuries nationwide. Thus, Park et al. concluded that the actual incidence of heat-related illnesses and injuries is about 50 times higher than reported (i.e., 170,000 ÷ 3,400 = 50). If the same ratio were applied to actual-versus-reported workplace fatalities – using the BLS’s officially reported 40 heat-related deaths per year – that would yield an estimate of 2,000 fatalities per year (i.e., 50 x 40 = 2,000). [Table 3]
Table 3: Estimated Annual Heat-Related Workplace Fatalities Derived From Ratio of Academic-to-Government Estimates on Total Heat-related Injuries
| Part 1: Calculate ratio of Park et al. to BLS estimate of heat-related workplace injuries. | Part 2: Apply Park et al. / BLS ratio on injuries to BLS estimate on heat-related workplace fatalities. | |||||
| Source of Workplace Injury Estimate | Estimated Injuries Attributable to Heat | Ratio Park et al. / BLS Estimate of Injuries | Park / BLS Ratio | BLS Fatality Estimate | Updated Estimated Total of Heat-related Fatalities | |
| Park et al. | 170,000 | 50:1 | 50 x 40 = 2,000 | |||
| BLS | 3,400 | |||||
According to official BLS data, there are about 5,000 on-the-job deaths each year across all categories of causes. In 2020, the most recent year for which data is available, the total was 4,764. The category accounting for the most fatalities that year was “Transportation,” at 1,778. “Exposure to harmful substances or environments,” the heading under which the subcategory of heat-related causes falls, was reported to account for 672 deaths.
Our estimates, above, place the number of occupational fatalities from environmental heat, alone, at 605 to 2,000 a year. At the low-end of this spectrum, deaths from environmental heat would rank fourth among discrete causes of workplace fatalities in 2020. At the high-end, environmental heat would rank as the number one cause of occupational fatalities. [Table 4]
Table 4: Causes of Workplace Fatalities Published by BLS, 2020
| Event or Exposure† | Cases |
| Roadway incidents involving motorized land vehicle | 1,038 |
| Intentional injury by person | 651 |
| Falls to lower level | 645 |
| Struck by object or equipment | 468 |
| Exposure to other harmful substances | 448 |
| Pedestrian vehicular incident | 330 |
| Non-roadway incident involving motorized land vehicles | 206 |
| Caught in or compressed by equipment or objects | 142 |
| Falls on same level | 136 |
| Exposure to electricity | 126 |
Source: Bureau of Labor Statistics
† BLS fatality records are broken into seven broad categories that carry one-digit codes. Under those categories are discrete causes of fatalities that carry two-digit codes, with subsets of causes listed under subordinate three-digit and four-digit codes. In 2020, the BLS reported at least one fatality pursuant to 22 two-digit categories. The top 10 such causes of fatalities are listed in Table 4. The category “Exposure to environmental heat” carries a three-digit code, listed under “Exposure to temperature extremes.”
As with our estimates on heat-related injuries and illnesses, our estimate on heat-related fatalities is imprecise. We do not know, for instance, if the California study accurately calculated the true number of heat-related injuries occurring annually or if the ratios of reported versus actual cases of fatalities would be the same as for injuries.
What we do know is that even at the official number of 40 per year, heat-stress accounts for an unacceptable number of fatalities. We also know that the officially reported 40 deaths per year represents a huge undercount compared to reality, as OSHA has recognized.
The actual number of heat-related occupational deaths is probably somewhere between 40 and 2,000 per year. Wherever the number lies, OSHA is obliged to take action to lower it.
B. Studies Consistently Associate Higher Temperatures With Workplace Injuries (as distinct from illnesses)
As mentioned above, one of the reasons that the BLS data fails to provide a true measure of workplace injuries is because it does not take into account the effect of high temperatures causing injuries, as distinct from illnesses. Research has shown that hotter temperatures increase fatigue and adversely affect cognitive performance,[41] decision-making,[42] and balance and motor skills.[43] Heat illnesses cause a wide range of symptoms that can limit an individual’s ability to safely carry out work functions such as dizziness, weakness, irritability, excessive sweating, muscle cramps and fainting. It goes without saying that these physical and mental effects of heat strain can cause falls and mistakes in the use of kitchen equipment, cutting tools, power tools, conveyor belts, pesticides and dangerous machinery. Many studies have looked at the correlation between temperatures and injuries.
A meta-analysis of 17 studies worldwide also showed an average 1% increase in occupational injuries for every 1 degree C above 20.9 degrees C (69.6 degrees F). Increases were highest, up to 1.7% increase in injuries per 1 degree C, in humid subtropical climates, such as the southeastern parts of the U.S.[46] A study of agricultural workers in Washington State found the odds of traumatic injuries in cherry harvesters, primarily from ladder falls, increased 1.53% for every 1 degree C above 25 degrees C (77 degrees F).[47]
Overnight low temperatures have an impact on heat-related injuries as well. Our natural bodily cooling systems are heavily strained on a very hot day. Those systems need to cool down and recover overnight.[48] A home without air conditioning or adequate ventilation can hinder the necessary bodily cooling, lessening the body’s ability to manage heat strain the next day and increasing susceptibility to heat-related illness.[49] The overnight heat may also increase workplace injuries by interrupting sleep and decreasing vigilance the following day.[50] A study of 47,000 workers’ compensation claims in Australia between 2002 and 2012 found a 1% increase in all acute injuries that resulted in 10 or more days of absence from work or high medical costs for every 1 degree C increase in daily minimum temperatures — overnight lows the night before the injury.[51]
Interestingly, studies have also shown a significant increase in acute occupational injuries occurring up to two days after the high heat exposure day,[52] including a study of nearly 2.3 million workers’ compensation claims in Italy between 2006 and 2010.[53] There is little research on the lingering effects of working under high heat stress; however this finding alludes to the possibility of heat stress symptoms continuing longer than one day and potentially causing injuries in following days.
III. Worker Heat-Stress Tragedies Disproportionately Strike Workers Who Are Poor, Black or Brown
The dangers of occupational heat stress are overwhelmingly borne by low-income workers, with the lowest-paid 20% of workers suffering five times as many heat-related injuries as the highest-paid 20%.[54]
Heat stress also disproportionately burdens workers of color. A recent review by Columbia Journalism Investigations of records relating to workplace heat injuries — including workplace inspection reports, death investigation files, depositions, court records, and police reports — found that since 2010, Hispanics/Latinos[55] have accounted for a third of all heat-related fatalities, despite representing only 18% of the U.S. workforce.[56]
These disproportionalities are visible in state datasets as well. In Washington state, an analysis of workers’ compensation claims found that while only 13% of the overall racial/ethnic composition of the state’s workforce in 2017 was Latino, they accounted for 21% of the claims for heat-related illness.[57] Similarly, while 4% of the population was Black, they accounted for 8% of the heat-related illness claims.[58]
The fact that workers who experience the highest rates of heat illness are disproportionately Hispanic/Latino or Black is largely due to the fact that these workers are over-represented in occupations that expose them to high levels of heat. About 30% percent of U.S. workers are Black or Hispanic/Latino but these workers account for about 40% of outdoor workers.
They make up more than 50% of laundry and dry-cleaning workers, cooks, dishwashers, industrial truck and tractor operators, telecommunications line installers and repairers, warehouse and storage workers, brick masons and cement masons. They account for about 65% of roofers.[59] Practitioners of these industries are at higher-than-normal risk of complications from heat stress. [Figure 1]
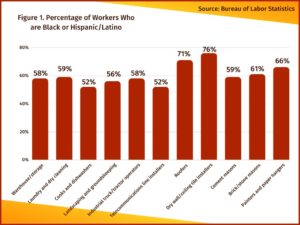
Hispanics make up approximately 78% of farmworkers nationwide,[60] and more than 90% in California.[61] While farmworkers suffer a strikingly high number of heat-related fatalities, the impact of ethnicity goes beyond over-representation in this highly risky occupation. Even within the agriculture industry, Hispanics die at a rate 3.5 times higher than non-Hispanics.[62]
Similarly, Black construction workers are 51% more likely to die from heat exposure than construction workers as a whole.[63] Mexican-born construction workers born are 91% more likely to die from heat exposure than the average of all construction workers.[64]
IV. Workers in Certain Industries, Such as Agriculture and Construction, Are at Extreme Risk of Harms from Unsafe Heat
As is the case for people of different demographic profiles, occupational risks fall unevenly on Americans based on their occupations. Those most at risk perform work that involves physical labor, often, though not exclusively performed outdoors.
A. Agricultural Workers
Agriculture workers die from heat stress at a rate 35 times greater than the rest of the U.S. workforce.[65]
Heat stress risk is exacerbated by structural vulnerabilities faced by farmworkers, including the fact that 70% of agricultural workers are foreign-born, and only 56% are legally authorized to work in the U.S.[66] Workers who are not authorized to work in the U.S. have almost no leverage to insist on adherence to proper workplace standards. Further, nearly a quarter of agriculture workers hold H-2A visas, temporary visas that make them rely on an employer’s sponsorship.[67] This dependence gives such employees little ability to demand safe working conditions.
Migrant farmworkers are particularly vulnerable to heat-related illness and injury.[68] The nature of their working conditions is exacerbated by cultural and language barriers, food insecurity, high poverty, and often substandard living conditions in labor camps and employer-provided housing.[69] Unfortunately, it is common for employer-provided housing to lack air conditioning or even fans.[70] A lack of basic health services and social support increases the chances that heat illness and injury go untreated.
To protect workers from heat illness, dehydration, and kidney injury, workers must drink plenty of water. Unfortunately, migrant farmworkers may not have sources of clean drinking water at home, and many employers may not provide it either.[71] Adequate clean, safe and easily accessible bathroom facilities with hand-washing stations are also essential to maintain worker hydration.[72] Without this kind of access, workers may intentionally reduce water intake in order to avoid the need to urinate.[73] The problem is exacerbated for women workers as sexual harassment and sexual assault may be more likely to occur near bathroom facilities in unsafe locations.[74]
In addition, many agricultural employers utilize payment structures — such as piece-rate payment (in which workers are paid based on the amount of crops they pick) – that push employees to work harder and minimize breaks out of a concern for lost wages.[75] Piece-rate pay systems may discourage workers from drinking necessary water or force workers to take drastic and humiliating measures like wearing diapers to avoid stopping for bathroom breaks.[76]
There is a growing body of evidence that heat stress is linked to both acute kidney injury and chronic kidney disease in farmworkers.[77] Heavy sweating from difficult manual labor in the sun can cause the body to lose dangerous amounts of water. Without adequate replacement, acute kidney injury can occur, which can lead to kidney failure or chronic kidney disease. Muscle damage due to heat-induced rhabdomyolysis, and toxins, such as pesticides and contaminated drinking water, are also contributing factors to kidney disease.[78]
It is estimated that, due to their outdoor jobs, 2.3 million U.S. workers are at risk for acute kidney injury or chronic kidney disease.[79] As many as one-third of migrant farmworkers in the U.S. experience acute kidney injury.[80] One study found a 47% increase in the likelihood of acute kidney injury among migrant farmworkers in Florida for every 5 degrees increase in heat index.[81] And a meta-analysis of heat stress in migrant farmworkers found piece-rate work to be significantly associated with kidney disease.[82]
The poor working and living conditions for farmworkers reflect both social injustice and racial/ethic injustice. The myriad issues facing these workers is inextricably entangled with inhumane and irrational immigration policies. Their vulnerability makes the protection of OSHA critical for these workers.
B. Construction Workers
Construction workers make up about 6% of the U.S. workforce, but they accounted for 36% of the total heat-related deaths across all industries between 1992 and 2016, as reported by the BLS.[83]
The construction industry has the second highest heat-related fatality rate. The industry itself is remarkably diverse with a wide range of trades and skill sets. Some jobs leave workers much more vulnerable to heat stress than others due to differences in heavy manual labor, cooling opportunities and exposure to radiant heat sources (e.g., direct sunlight, asphalt, concrete, machinery), among other factors. Cement masons have the highest fatality rate, 10 times the rate of construction workers broadly.[84] The heat-related fatality risks for roofers and construction helpers are nearly seven times that of the general industry.[85] Brick masons, construction laborers and heating/air conditioning/refrigeration mechanics also have higher than average heat-related fatality risks when compared to construction workers as a whole.[86]
The common presence of dangerous machinery and tools in construction workplaces, as well as working on roofs and scaffolding, increase the chance of heat-related injuries from accidents and falls. Many construction workplaces also put workers in close proximity to dangerous chemicals and solvents which create a unique risk of heat-related illness. Heat stress can increase worker susceptibility to these agents by increasing absorption rates and toxicity.[87]
C. Indoor Workers
While heat stress is often associated with outdoor jobs such as farming and construction, indoor workers are also at risk from dangerously high temperatures. Indoor heat stress is prevalent in enclosed workplaces or workplace sections without climate control or adequate ventilation. It’s also common in workplaces with heat-generating machinery like ovens, kilns, and machinery for making textiles, among many others. Obviously, indoor heat stress can be a problem year-round. Common workplaces that experience high indoor temperatures all year round include warehouses, factories, electrical utilities, bakeries, commercial kitchens, laundries, chemical plants, glass manufacturers and metal refineries/ foundries.[88]
The complaints to Oregon OSHA during the June 2021 heat wave reveal an interesting, perhaps unexpected, pattern — the vast majority of the complaints were about indoor heat. Of the 116 heat-related complaints filed with Oregon OSHA from June 24 to June 30, 2021, 91 described inadequate protections for excessive indoor heat.[89] This is a remarkable 5.7 times the number of complaints filed against employers for inadequate protections for outdoor workers — only 16 complaints were filed against outdoor employers. [Figure 2]
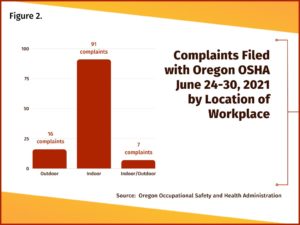
For example, restaurant workers had to meet dramatically higher service demands as the public tried to evade the heat by avoiding the use of stoves and ovens in their own homes.[90] Unfortunately, this left restaurant workers to labor at high speeds and swelter in the heat created by the workplace cooking equipment combined with inadequate cooling from strained air conditioners.
D. First Responders
Climate-induced and heat-related fires put large numbers of firefighters and rescue personnel in danger of serious heat stress, complicated by smoke inhalation, as they risk their lives to protect others. For example, on a single day in August 2021, more than 13,500 firefighters warred with California wildfires.[91]
Other first responders, like police officers and ambulance drivers, have to cope with critical heat-related emergencies, as well. For example, first responders have to manage urgent heat-related health emergencies and heat strokes that increase during heat waves and high heat days.[92] With increasing wildfires, victims of fire, heat and smoke inhalation need urgent medical care, while wildfire evacuations require police management. The work of first responders can be made even more dangerous when combined with other extreme weather associated with climate change, like strong storms that cause flash flooding.[93] And as global warming continues, these trends will be exacerbated.[94]
E. Infrastructure and Utility Workers
Heat waves can create public needs that require workers to devote long hours in the heat, often working at a very fast pace with little or no breaks. HVAC employees have to work long hours trying to meet the needs of customers who require urgent repairs to air conditioning units and installation jobs also increase.[95] Utility workers may have to respond to power outages caused by overextension of the energy grid due to high air-conditioning use.[96] During the 2021 heat wave in the Pacific Northwest, road workers, rail workers and construction laborers had to provide a quick response to repair the buckled roads and melted railway and streetcar power cables in Portland that crippled public transportation.[97]
V. Workers at Risk of Suffering Heat-Related Injuries Are Much Less Likely to Have Health Insurance or Qualify for Workers’ Compensation
Many of the workers most exposed to excessive heat on the job lack health insurance or access to workers’ compensation. This both leaves workers vulnerable to financial catastrophe from injuries and illnesses caused by on-the-job heat and increases the likelihood that an easily treatable condition will progress to a more serious illness or death.
States have different rules about when employers are required to have workers’ compensation insurance and which workers it must cover.[98] These rules often leave the workers that are most susceptible to heat-related illness, injury and death without access to workers’ compensation benefits. For example, employers are exempt from providing workers’ compensation for farmworkers in 16 states.[99] And, as already noted, more than a third of farmworkers are undocumented.[100] While many state laws require workers’ compensation benefits for undocumented workers, many state laws do not.[101] And Texas doesn’t require non-governmental employers to have workers’ compensation insurance at all.[102]
Another large gap in workers’ compensation benefits for workers in occupations with significant heat hazards is an exemption for casual workers and independent contractors.[103] Casual workers are defined by their limited relationship to the employer. They often include day laborers and temporary helpers, [104] roles commonly seen in construction and seasonal outdoor employment. Workers classified as independent contractors receive no workers’ compensation benefits from the employer who hired them.
Many workers categorized as independent contractors might be miscategorized. Definitions of what constitutes an independent contractor vary from state to state. [105] And in many states, those definitions are hazy or not adhered to. This has led to a great deal of confusion and, because employers generally have a financial incentive to categorize a worker as an independent contractor, there is a lot of misclassification. The problem is particularly prevalent in the construction industry.[106] A study finding that only 5% of injured construction workers had their medical expenses covered by workers’ compensation also found that a third of the construction workers were improperly classified as independent contractors.[107]
Even when workers have access to workers’ compensation, they may have difficulty receiving benefits for heat-related illnesses and injuries. An employee must show that a heat-related illness or injury occurred at work. Unless an employee collapses at work or is sent for medical treatment directly from the workplace, that can be difficult to prove. As has been discussed above, some acute conditions may be a delayed response to heat stress. Heat stress often triggers other illnesses and injuries such as a heart attack or kidney failure.[108] The medical treatment and records may neglect the role of excessive heat in precipitating the condition being treated.[109]
All of these issues make it less likely that workers, or their families, will be able to demonstrate that the illness, injury, disability, or even death was due to excessive heat conditions on the job. Unfortunately, the concern that the cost of health care may not get covered by workers’ compensation may discourage workers from seeking the medical help they need for injuries or conditions that may lead to dangerous complications over time.
Given the limited protection offered by workers’ compensation, it’s especially critical that workers have health insurance. Unfortunately, many of those with high heat hazard jobs lack access to affordable insurance or care.[110] Only 48% of farmworkers have health insurance, a number that drops to 41% for migrant farmworkers and 22% for unauthorized workers.[111] There is a racial disparity in health care use, as well.
Lack of health insurance is a big problem across the construction industry. Of the 20 occupations in the United States least likely to have health insurance, 11 of them are occupations in the construction industry, including the the top five jobs with the highest heat-related death rates within the industry — cement masons (39% uninsured), roofers (50.5% uninsured), brick masons (39% uninsured), construction laborers (37.5% uninsured) and construction helpers (43% uninsured).[112] [Figure 3]
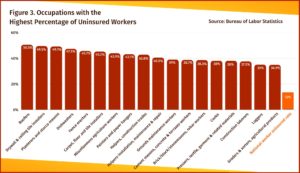
Workers navigating high heat in commercial kitchens also make it into the top 20 jobs least likely to have health insurance, specifically cooks (38% uninsured) and dishwashers (47% uninsured).[113] Nearly 38% of ironing and pressing machine operators have no health insurance.[114] Grounds maintenance workers and loggers make it into the top 20 least insured occupations as well, with uninsured rates of 39% and 35%, respectively.[115]
VI. Why OSHA Should Issue an Interim Heat Standard and What Should Be in It
Fifty years ago, the National Institute for Occupational Safety and Health (NIOSH) studied the effects of heat stress on workers and recommended that OSHA adopt an occupational heat standard. But OSHA has never done so.
Last year, in response to a petition submitted by Public Citizen and more than 100 other groups, OSHA finally began working on a heat-safety standard.[116] But the process for creating new safety standards has become so cumbersome that it now takes the agency an average of eight years to complete one, and can take far longer.[117]
This theoretically leaves OSHA with two choices to protect workers before a permanent standard is adopted. The first is to rely on its General Duty Clause, which calls for employers to furnish their employees with conditions that are free of hazards “that are causing or are likely to cause death or serious physical harm to his employees.” But this is not practical. Taking enforcement action pursuant to the General Duty Clause is time-consuming and often vulnerable to legal challenges. In fact, an Administrative Law Judge and the full Occupational Safety and Health Review Commission, in recent years, have thrown out several attempts by OSHA to sanction employers under the General Duty Clause for subjecting their employees to unacceptable risks due to heat.[118]
A second option would be for OSHA to create an Emergency Temporary Standard (ETS). An ETS can be created and adopted in months and carries the same force as a permanent standard. A limitation regarding an ETS is that it only lasts for six months. It has not been determined if OSHA would be able to extend an ETS in a situation in which a hazard remains and a permanent standard under development is not finalized. Nonetheless, the agency should issue an emergency standard as soon as possible to address the crisis of the moment, and figure out how to deal with possible challenges to the standard’s duration or extension if they arise.
A. Conditions Justify Creating an Emergency Temporary Standard to Protect Workers From Heat Stress
To issue an Emergency Temporary Standard (ETS), OSHA must determine that workers are being exposed to a grave danger and that adequate evidence exists that an ETS is necessary to protect workers from such danger.[119]
These are not difficult hurdles to clear. Heat stress kills workers. All occupational heat-related deaths are preventable and an effective and enforced heat ETS will unquestionably save lives.
Two states have already found a critical need to issue emergency temporary standards. In direct response to the fatal June 2021 Pacific Northwest heat wave, both Oregon and Washington adopted emergency temporary heat standards.[120] As Andrew Stolfi, director of the Oregon Department of Consumer and Business Services, which includes Oregon OSHA, said, “In the face of an unprecedented heat wave in the Pacific Northwest – and tragic consequences – it is absolutely critical that we continue to build up our defenses against the effects of climate change, including extreme heat events.”[121]
He went on to say that “the risks of working in high heat are not going away this, or any, summer.”[122] Speaking about the heat standard that Washington already had in place prior to issuing the new emergency temporary heat standard Gov. Jay Inslee said, “The real impacts of climate change have changed conditions since those rules were first written and we are responding.”[123]
The new normal of fatal heat waves and record-breaking summers poses a grave danger to workers. While high temperatures have always posed a potentially fatal hazard to workers, the problem is rapidly intensifying. OSHA agrees. The agency has stated that “workplace exposure to heat is a significant hazard and will become more critical as the impacts of climate change progress over time.”[124]
Given our changed reality of deadly, record-breaking heat waves every summer,[125] increasing extreme heat days,[126] and the tragic death tolls they produce, there is substantial and compelling evidence that occupational heat exposure poses a grave danger to workers.
B. An Emergency Temporary Standard Will Reduce The Grave Danger Of Occupational Heat Illness And Injury
Recent research on heat-related injuries in California from 2001 to 2018 found that the increase in injuries on hot days was cut by approximately 30% in the years following California’s issuance of a state occupational heat standard in 2005.[127] This clearly demonstrates the potential for a federal heat rule to significantly reduce the effects of heat on worker safety and health.
Based on the results in California, a federal ETS similar to California’s heat standard would prevent more than 50,000 heat-related injuries annually. Since California’s limited standard only covers outdoor workplaces and exempts numerous industries from implementing high-heat procedures,[128] a strong federal standard covering both outdoor and indoor workplaces could prevent significantly more injuries and fatalities. The high number of preventable heat-related injuries easily demonstrates a necessity for a heat ETS.
C. Recent Rulings Cast Doubt on OSHA’s Ability to Protect Workers in the Absence of an Occupational Heat Standard
While OSHA can cite companies for heat exposure violations under its General Duty Clause, several rulings of the Occupational Safety and Health Review Commission (OSHRC), an administrative court, since 2018 demonstrate that the lack of a standard specifically focused on heat hinders OSHA’s ability to hold employers accountable for dangerous heat hazards. For example, an OSHRC Administrative Law Judge (ALJ) issued five substantially identical decisions in similar cases in which OSHA alleged the United States Postal Service, in multiple locations, exposed its employees to unmitigated excessive heat as they delivered the mail.
In each case, the ALJ vacated OSHA’s citation, finding that OSHA had not met its burden to establish that a condition in the workplace presented a hazard, even in the face of evidence of heat indices as high as 109 degrees and workers medically diagnosed with heat illnesses.[129]
The ALJ, noted that “without a temperature- or heat index-specific standard, it is difficult for employers to know when heat is ‘excessive,’”[130] and referenced OSHA’s failure to provide such a standard, stating, “OSHA has been urged to promulgate a heat stress standard since shortly after the [OSH] Act went into effect.”[131] Due to legal precedent and given the absence of a standard, the ALJ stated that it is “difficult to establish” that excessive heat is a cognizable hazard under the general duty clause.[132]
D. What Should Be in an Emergency Temporary Standard to Protect Workers from Heat Injury, Illness and Death
Every workplace injury and fatality caused by heat stress is avoidable, and relatively simple preventative measures have proven extremely effective at protecting workers. It is both the social and legal responsibility of employers to create a work eenvironment safe from heat hazards.
OSHA should create an Emergency Temporary Standard delineating required preventative measures that include the following:
Temperature Thresholds: An OSHA heat standard must provide clarity to employers and workers in order to ensure effective comprehension and implementation of the standard. This is particularly important for small businesses, where reliance on complicated formulas for decision-making may be cumbersome. Identifying clear temperature thresholds that trigger certain minimum employer requirements under the standard will protect both workers and employers.
Workload and Pace: Employers should empower workers to work at their own pace whenever possible. Workload should be reduced or suspended in times of extreme temperatures.
Mandatory Rest breaks: Employers should be required to give workers a 15-minute break for every two hours of work when the temperature exceeds 80 degrees. Scheduled breaks should increase with temperatures based on the work/rest schedule recommended by NIOSH with a clothing adjustment. Workers should be permitted and encouraged to take unscheduled breaks when they feel overheated or experience any symptoms of heat illness.
Indoor and Outdoor Cooling: Indoor workplaces should be air-conditioned or well-ventilated to keep temperature below 80 degrees. Or, at a minimum, include a cool space for breaks. Delivery trucks should be air conditioned whenever possible. Outdoor workplaces should provide a cool space for breaks.
Hydration: Employers should be required to provide workers at least one liter of cold drinking water every hour. Water should be easily accessible and, preferably made continuously available. With very heavy workloads at high temperatures workers also should be provided drinks with electrolytes.
Heat Stress Plan: Each employer should use the information available from OSHA, NIOSH, industry-specific guidance and other expert sources to create a written heat stress plan that is appropriate for use at their unique worksites. The plan should be comprehensive and available to employees in a language they can understand.
Emergency Response: Employers should be required to have an emergency action plan (EAP) that includes training personnel to identify workplace heat illnesses and to provide appropriate cooling strategies at each worksite. Designated employees or managers should be trained in specific workplace medical responses. The EAP should include information on when to call an ambulance, including guidance to call an ambulance when in doubt.
Heat Acclimatization Plan: All workers beginning work in high-heat environments, or who will be working in hotter conditions than usual (e.g., during a heat wave), must be gradually acclimatized to the work over a period of at least 7 to 14 days.
Environmental Surveillance and Hazard Notification: At outdoor worksites, employers should be required to monitor environmental conditions at each worksite and notify. employees of hazardous heat conditions in English and any languages spoken by at least 20% of workers.
Worker Information and Training: Employers must be required to provide all employees with heat stress training when they are hired, as well as annually in the employees’ primary language.
Record Keeping: Employers should be required to maintain and properly handle accurate records of 1) heat illnesses, including those treated onsite with first aid; 2) accidents or injuries potentially related to heat strain, including recording the workplace temperature and protective clothing worn by the worker for every workplace injury; 3) environmental and metabolic heat exposures; 4) acclimatization procedures; 5) all medical and physiological monitoring; and 6) modifications to engineering and administrative controls, as well as changes to personal protective equipment.
Non-retaliation Policy: Workers should be vigorously protected from all forms of employer retaliation for reporting unsafe conditions that could lead to heat illness or injury. An OSHA heat standard must include comprehensive whistleblower rights.
Conclusion
Workers are facing unacceptable risks due to soaring temperatures. It is OSHA’s duty to ensure that workers are provided with safe conditions. The solutions to protect workers from dangerous temperatures are simple. OSHA must take action immediately to ensure that employers follow these commonsense steps.
[1] Assessing the Global Climate in 2021, National Oceanic and Atmosphere Administration (NOAA), National Centers for Environmental Information (Jan. 13, 2022), https://bit.ly/3QgFNo7.
[2] State of the Climate: Monthly Global Climate Report for February 2022, NOAA, National Centers for Environmental Information (March 2022) (accessed on June 7, 2022), https://bit.ly/3x8SmsK.
[3] June 2021 Was the Hottest June on Record for U.S., NOAA (July 9, 2021), https://bit.ly/36EOwLe.
[4] Chris Dolce, Summer 2021 Was the Hottest on Record in the Contiguous U.S., NOAA Says, Weather.com (Sept. 9, 2021), https://bit.ly/31z5oUr. Assessing the U. S. Climate August 2021, NOAA (Sept. 9, 2021), https://bit.ly/NOAA921.
[5] It’s Official: July Was Earth’s Hottest Month on Record, NOAA (Aug. 13, 2021), https://bit.ly/3ASejfS.
[6] Aatish Bhatia and Winston Choi-Schagrin, Why Record-Breaking Overnight Temperatures Are So Concerning, Nights Are Warming Faster Than Days Across Most of The U.S., With Potentially Deadly Consequences, The New York Times (July 22, 2021), https://nyti.ms/3jjDmCs.
[7] Climate Change Indicators: Heat Waves, U.S. Environmental Protection Agency (EPA) (accessed on June 22, 2022), https://bit.ly/3y3AI87. In this analysis, a heat wave is defined as two or more consecutive days when the daily minimum heat index (overnight lows) exceeds the 85th percentile of historical July and August temperatures (1981–2010) for that area.
[8] Jason Samenow and Ian Livingston, Canada Sets New All-Time Heat Record of 121 Degrees Amid Unprecedented Heat Wave, Washington Post (June 29, 2001), https://wapo.st/3mzVkS7.
[9] Dora Totoian, Farmworker Dies in Willamette Valley Record Heat, Statesman Journal (June 29, 2021), https://bit.ly/3x7EhKX; Morgan Romero, Oregon OSHA Investigating Death of Walmart Warehouse Worker in Hermiston, KGW8 (July 9, 2021), https://bit.ly/3raw0Ut; Monica Samaha, Hillsboro Construction Worker Latest Workplace Heat Death, Oregon Public Broadcasting (July 21, 2021). https://bit.ly/3jk5LZb; Amelia Templeton and Monica Samayoa, Oregon Medical Examiner Releases Names of June Heat Wave Victims, Oregon Public Broadcasting (Aug. 6, 2021), https://bit.ly/3sRoMpi.
[10] IPCC, 6th Assessment Report (2021).
[11] Top 20 Largest California Wildfires, Cal Fire (accessed May 13, 2022), https://bit.ly/3Pjx43M.
[12] What’s Behind California’s Surge in Large Fires?, NASA’s Earth Observatory (Sep. 13, 2021), https://go.nasa.gov/37M2ZZW.
[13] Criteria for a Recommended Standard: Occupational Exposure to Hot Environments, Revised Criteria, National Institute of Occupational Safety and Health (February 2016), https://bit.ly/3e4AjeG [hereinafter NIOSH Recommended Heat Standard (2016)].
[14] NIOSH Recommended Heat Standard (2016).
[15] See, e.g., Chin Leong Lim, Fundamental Concepts of Human Thermoregulation and Adaptation to Heat: A Review in the Context of Global Warming, 17 International Journal of Environmental Research and Public Health 7795 (Oct. 24, 2020), https://bit.ly/2XTy5d1.
[16] Id.
[17] NIOSH Recommended Heat Standard (2016).
[18] Heat Stress – Heat-Related Illness, Centers for Disease Control and Prevention (CDC) (accessed on June 22, 2022), http://bit.ly/3fqShJi.
[19] Id.
[20] See, e.g., Sally Moyce, Dianne Mitchell, Tracey Armitage, Daniel Tancredo, Jill Joseph and Marc Schenker, Heat Strain, Volume Depletion and Kidney Function in California Agricultural Workers, 74(6) Occupational and Environmental Medicine 402-409 (Jan. 19, 2017), https://bit.ly/2Z7Psal [hereinafter Moyce et al., Kidney Function in California Agricultural Workers (2017)]; Andreas D. Flouris, Petros C. Dinas, Leonidas G. Ioannou, Lars Nybo, George Havenith, Glen P. Kenny and Tord Kjellstrom, Workers’ Health and Productivity Under Occupational Heat Strain: Systematic Review and Meta-Analysis, 2(12) The Lancet Planetary Health E521-E531 (Dec. 1, 2018), https://bit.ly/3DRPl2z.
[21] Moyce et al., Kidney Function in California Agricultural Workers (2017).
[22] Elizabeth Rogers, The Survey of Occupational Injuries and Illnesses Respondent Follow-Up Survey, Monthly Labor Review, Bureau of Labor Statistics (May 2020), https://bit.ly/2UukCqo. This raises obvious concerns not only about the accuracy of data, but also the oversight of employer record-keeping on workplace injuries. Reliance on voluntary compliance with OSHA rules clearly has limitations.
[23] Heat, Related Standards, OSHA (accessed on June 22, 2022), https://bit.ly/3z5CB5x.
[24] Nonfatal Cases Involving Days Away from Work: Selected Characteristics (2011 forward), BLS (accessed June 7, 2022), https://bit.ly/38YK8LP. Annual estimates were retrieved by selecting Area — “All U.S.,” Ownership — “All ownerships,” Data Type — “Injury and illness cases,” Case type — “Industry division or selected characteristic by detailed event or exposure,” Category — “00X All Industry,” and Event or Exposures — “531XXX Exposure to environmental heat.”
[25] Census of Fatal Occupational Injuries (2011-forward), BLS (accessed June 7, 2022), https://bit.ly/3NzjvvV. Annual estimates were retrieved by selecting Area — “All U.S.,” Case type — “Fatalities in all sectors,” Category — “E5A Event or exposure — exposure to environmental heat,” and Industries — “000000 All Workers.”
[26] Heat Injury and Illness Prevention in Outdoor and Indoor Work Settings, 86(205) Federal Register 59309 (Oct. 27, 2021), https://bit.ly/3dosuj7.
[27] R. Jisung Park, Nora Pankratz & A. Patrick Behrer, Temperature, Workplace Safety, and Labor Market Inequality, IZA Institute of Labor Economics DP No. 14560 3 (July 2021), https://bit.ly/2V3WriI [hereinafter R. Jisung Park et al., Temperature, Workplace Safety, and Labor Market Inequality (2021)].
[28] The California climate varies greatly and is a useful, though imperfect, representation of the worker population in other states. The geography of the state incudes all five climate zones found in the continental U.S. — Tropical, Dry, Moist Subtropical Mid-Latitude, Moist Continental Mid-Latitude and Highlands. Jet Stream Climate Zones, National Weather Service, NOAA (accessed on June 21, 2022), https://bit.ly/3zRTZ0V. Moreover, the response to environmental heat is relative to the typical heat for the location.
[29] According to BLS, the U.S. civilian labor force as of June 2021 was 162.167 million, approximately 8.58 times larger than California’s civilian labor force as of June 2021 of 18.89 million. Multiplying California’s 20,000 heat-related injuries by 8.58 equals 171,696 estimated heat-related injuries nationally (162.167 million U.S. workers / 18.89 million CA workers x 20,000 CA heat-related injuries = 171,696 heat-related injuries nation-wide). Note that this figure assumes the number of California injuries attributed to hot days is representative of the entire U.S. While the average number of hot days in the U.S. varies, the same is true of California. See, e.g., Average Number of Hot Days at U.S. Cities in Summer, Current Results —Weather and Science Facts (accessed on June 23, 2022), https://bit.ly/3bp90xf.
[30] Census of Fatal Occupational Injuries (2011-forward), BLS (accessed June 7, 2022), https://bit.ly/3NzjvvV. Annual estimates were retrieved by selecting Area — “All U.S.,” Case type — “Fatalities in all sectors,” Category — “E5A Event or exposure — exposure to environmental heat,” and Industries — “000000 All Workers.” Injuries/Illnesses and Fatal Injuries Profiles, BLS (accessed June 7, 2022), https://bit.ly/3tmE9HJ. Annual estimates were retrieved for 1992-2002 by selecting Table type — “Fatal Injuries Numbers,” Year — “2002,” Area — “All U.S.,” Beginning Year — “1992,” Characteristic type — “Event or exposure,” Order — “Numeric,” Subcharacteristic — “321XXX Exposure to environmental heat,” Ownership — “All ownerships.” The procedure was repeated for 2003-2010.
[31] The BLS Census of Occupational Injury (CFOI) collects multiple source documents, because each work-related death must be confirmed by at least two sources. Of the source documents collected, death certificates are collected on all deaths and medical examiner/autopsy/coroner reports are commonly collected. Other sources may serve as confirmation, such as toxicology, OSHA or workers’ comp reports, and even the news media. Census of Fatal Occupational Injuries: Data Sources, BLS (accessed on June 12, 2022), https://bit.ly/3OcqN8U. The CFOI examines all cases where the death certificate is marked “At work” and, additionally, occupational illness reports from OSHA to determine if there was an injury component to the illness. Scope of the Census of Fatal Occupational Injuries (CFOI), BLS (accessed on June 13, 2022), https://www.bls.gov/iif/cfoiscope.htm
[32] Technical Documentation: Heat Related Deaths, Environmental Protection Agency (accessed on June 8, 2022), https://bit.ly/3mvfRY5.
[33] Ambarish Vaidyanathan, Josephine Malilay, Paul Schramm and Shubhayu Saha, Heat-Related Deaths — United States, 2004–2018, 69 Morbidity and Mortality Weekly Report (MMWR), CDC 729–734 (2020), https://bit.ly/3mSwWLX.
[34] Climate Change Indicators: Heat-Related Deaths, Environmental Protection Agency (EPA) (web update: April 2021) (accessed on June 7, 2022), https://bit.ly/3y3AI87.
[35] Technical Documentation: Heat Related Deaths, EPA (accessed on June 8, 2022), https://bit.ly/3mvfRY5.
[36] Climate Change Indicators: Heat-Related Deaths, EPA (web update: April 2021) (accessed on June 7, 2022), https://bit.ly/3y3AI87.
[37] Kate Weinberger, Daniel Harris, Keith Spangler, Antonella Zanobetti and Gregory Wellenius, Estimating the Number of Excess Deaths Attributable to Heat in 297 United States Counties, 4(3) Environmental Epidemiology e096 (April 23, 2020), https://bit.ly/38bVp7D.
[38] Id.
[39] Multiplying 5,608 heat-related fatalities by 1.619 = 9,079, arriving at estimated heat-related fatalities nationally among the general population.
[40] Drew Shindell, Yuqiang Zhang, Melissa Scott, Muye Ru, Krista Stark and Kristi L. Ebi, The Effects of Heat Exposure on Human Mortality Throughout the United States, 4(4) GeoHealth e2019GH000234 (2021), https://bit.ly/3xmyxyj.
[41] Joshua Graff Zivin, Solomon Hsiang and Matthew Neidell, Temperature and Human Capital in the Short and Long Run, 5(1) Journal of the Association of Environmental and Resource Economists 77, 77-105 (2018), https://bit.ly/3NmdEJG.
[42] Anthony Heyes & Soodeh Saberian, Temperature and Decisions: Evidence From 207,000 Court Cases, 11(2) American Economic Journal: Applied Economics 238-265 (2019), https://bit.ly/3tV1a4G.
[43] Jacob F. Phil, Chris J. Mikkelsen, Nicklaus Junge, Nathan B. Morris and Lars Nybo, Heat Acclimatization Does Not Protect Trained Males from Hyperthermia-Induced Impairments in Complex Task Performance, 16(5) International Journal of Environmental Research and Public Health 716 (February 28, 2019), https://bit.ly/2X46s0p; Jacob F. Piil, Lasse Christiansen, Nathan B. Morris, C. Jacob Mikkelsen, Leonidas G. Ioannou, Andreas D. Flouris, Jesper Lundbye-Jensen and Lars Nybo, Direct Exposure of The Head To Solar Heat Radiation Impairs Motor-Cognitive Performance,10 Scientific Reports 7812 (May 2020), https://go.nature.com/3y0L0pF.
[44] R. Jisung Park et al., Temperature, Workplace Safety, and Labor Market Inequality (2021).
[45] Miriam M. Calkins, David Bonauto, Anjum Hajat, Max Lieblich, Noah Seixas, Lianne Sheppard and June T. Spector, A Case-crossover study of Heat Exposure and Injury Risk Among Outdoor Construction Workers in Washington State, 45(6) Scandinavian Journal of Work, Environment and Health 588-599 (2019), https://bit.ly/3D5Tkaq.
[46] Syeda Hira Fatima, Paul Rothmore, Lynne C. Giles, Blesson M. Varghese and Peng Bi, Extreme Heat and Occupational Injuries in Different Climate Zones: A Systematic Review and Meta-analysis of Epidemiological Evidence, 148 Environment International 106384 (Mar., 2021), https://bit.ly/3jGUEcL [hereinafter Fatima et al., Extreme Heat and Occupational Injuries in Different Climate Zones (2021).]
[47] June T. Spector, David K. Bonauto, Lianne Sheppard, Tania Busch-Isaksen, Miriam Calkins, Darrin Adams, Max Lieblich and Richard A. Fenske, A Case-crossover Study of Heat Exposure and Injury Risk in Outdoor Agricultural Workers, Plos One (Oct. 7, 2016), https://bit.ly/2ZQLxiz.
[48] Glen P. Kenny and Ryan McGinn, Restoration of Thermoregulation After Exercise, 122 Journal of Applied Physiology 933–944 (April 11, 2017), https://bit.ly/3fatYyt.
[49] Sean R. Notley, Robert D. Meade, Andrew W. D’Souza, Brian J. Friesen and Glen P. Kenn, Heat Loss Is Impaired in Older Men on the Day after Prolonged Work in the Heat, 50(9) Medicine and Science in Sports and Exercise 1859-1867 (September 2018), https://bit.ly/3NeUo0Y; Robert D. Meade, Andrew W. D’Souza, Lovely Krishen and Glen P. Kenny, The Physiological Strain Incurred During Electrical Utilities Work Over Consecutive Work Shifts in Hot Environments: A Case Report, 14(12) Journal of Occupational and Environmental Hygiene 986–994 (November 2017), https://bit.ly/3l8PvdL; Zachary J. Schlader, Deanna Colburn and David Hostler, Heat Strain Is Exacerbated on the Second of Consecutive Days of Fire Suppression, 49(5) Medicine and Science in Sports and Exercise 999-1005 (May 2017), https://bit.ly/3wxU8n8.
[50] Judith A. McInnes, Muhammad Akram, Ewan M. MacFarlane, Tessa Keegel, Malcolm R. Sim and Peter Smith, Association Between High Ambient Temperature and Acute Work-related Injury: A Case-crossover Analysis Using Workers’ Compensation Claims Data, 43(1) Scandinavian Journal of Work, Environment and Health 86-94 (2017), https://bit.ly/2ZNFxXR.
[51] Id.
[52] Fatima et al., Extreme Heat and Occupational Injuries in Different Climate Zones (2021).
[53] Alessandro Marinaccio, Matteo Scortichini, Claudio Gariazzo, Antonio Leva, Michela Bonafede, Francesca K. de’ Donato, Massimo Stafoggia, Giovanni Viegi Paola Michelozzi, Nationwide Epidemiological Study for Estimating the Effect of Extreme Outdoor Temperature on Occupational Injuries in Italy, 133(A) Environment International 105176 (Dec. 2019), https://bit.ly/3Gy8ZC8.
[54] R. Jisung Park et al., Temperature, Workplace Safety, and Labor Market Inequality (2021).
[55] Research and sources relied upon throughout this report use the terms Hispanic, Hispanic/Latino or Latino based on the terminology used by the database or research being discussed.
[56] Julia Shipley, Brian Edwards, David Nickerson, Robert Benincasa, Stella Chávez and Cheryl Thompson, Heat is Killing Workers in the U.S. — and There Are No Federal Rules to Protect Them, National Public Radio (Aug. 17, 2021), https://n.pr/3y0WAkC .
[57] Martell Hesketh, Sara Wuellner, Amanda Robinson, Darrin Adams, Caroline Smith and David Bonauto, Heat Related Illness Among Workers in Washington State: A Descriptive Study Using Workers’ Compensation Claims, 2006-2017, 63(4) American Journal of Industrial Medicine 300-311 (April 2020), https://bit.ly/3z57gjm.
[58] Id.
[59] Labor Force Statistics from the Current Population Survey, Bureau of Labor Statistics (2021), http://bit.ly/3bV3xvn.
[60] Findings from the National Agriculture Workers Survey (NAWS) 2019-2020: A Demographic and Employment Profile of United States Farm Workers, Research Report No. 16, JBS International, Inc., (June 3. 2022), https://bit.ly/3tnsvfy [hereinafter NAWS 2022]. The annual NAWS report is a multiagency effort, including The Department of Labor, the Department of Health and Human Services, the Department of Education and the Environmental Protection Agency, to obtain more thorough information on crop workers in the U.S. Using a less detailed methodology, BLS estimates a lower percentage of Hispanic/Latino crop workers. Most of the data in this report rely on BLS data.
[61] Kristina Dahl and Rachel Licker, Too Hot to Work: Assessing the Threat Climate Change Poses to Workers, Union of Concerned Scientists (Aug. 2021), https://bit.ly/3CXOQ6C.
[62] Id.
[63] Xiuwen Sue Dong, Gavin West, Alfreda Holloway-Beth, Xuanwen Wang & Rosemary Sokas, Heat-Related Deaths Among Construction Workers in the United States, 62(12) American Journal of Industrial Medicine 1047-1057 (Dec. 2019), https://bit.ly/3CWYd6J [hereinafter Dong et al., Heat-related Death in Construction Workers (2019)].
[64] Id.
[65] Diane Gubernot, Brooke Anderson & Katherine Hunting, Characterizing Occupational Heat-Related Mortality in the United States, 2000-2010: An Analysis Using the Census of Fatal Occupational Injuries Database, 58(2) American Journal of Industrial Medicine 203, 203-211 (Feb. 2015), https://bit.ly/3j2wV70.
[66] NAWS 2022.
[67] Farm Labor, USDA Economic Research Service (accessed June 9, 2022), https://bit.ly/3myZPMN.
[68] Moussa El Khayat, Dana A. Halwani, Layal Hneiny, Ibrahim Alameddine, Mustapha A. Haidar and Rima R. Habib, Impacts of Climate Change and Heat Stress on Farmworkers’ Health: A Scoping Review, 10 Frontiers in Public Health 782811 (February 2022), https://bit.ly/3yZASSf [hereinafter El Khayat et al., Impacts of Climate Change and Heat Stress on Farmworkers’ Health: A Scoping Review (2022)].
[69] Id.; See, also, Teresa Wiltz, States Struggle to Provide Housing for Migrant Farmworkers, Stateline, Pew Trusts (May 2, 2016), https://bit.ly/3NFxPmk.
[70] Farm Workers and the Environment, National Farm Worker Ministry (accessed on Jan. 10, 2022), https://bit.ly/3Gevmf3; Adam Wagner, Aaron Sánchez-Guerra and Nadia Ramlagan, With No AC Where They Sleep, NC Farmworkers Risk the Heat Even After the Sun Goes Down, Pulitzer Center (Oct. 21, 2020), https://bit.ly/3ndy2lE.
[71] El Khayat et al., Impacts of Climate Change and Heat Stress on Farmworkers’ Health: A Scoping Review (2022).
[72] Margaret C. Morrissey, Douglas J. Casa, et al., Heat Safety in the Workplace: Modified Delphi Consensus to Establish Strategies and Resources to Protect U.S Workers, 5(8) GeoHealth e2021GH000443 (August 2021), https://bit.ly/3Elttfk. While NAWS indicates that 99% of farmworkers have access to toilets and hand washing stations, immigrants and piece-rate workers less likely to have access. Anita Alves Pena and Edward R. Teather-Posadas, Field Sanitation in US Agriculture: Evidence from NAWS and Future Data Needs, 23(2) Journal of Agromedicine 123–33 (2018), https://bit.ly/3Ou1vmG.
[73] See, e.g., Leonidas G. Ioannou, Josh Foster, Nathan B. Morris, Jacob F. Piil, George Havenith, Igor B. Mekjavic, Glen P. Kenny, Lars Nybo and Andreas D. Flouris, Occupational Heat Strain in Outdoor Workers: A Comprehensive Review and Meta-analysis, 9(1) Temperature 67-102 (April, 2022), https://bit.ly/3yxAQ3K [hereinafter Ioannou et al., Heat Strain Comprehensive Review and Meta-Analysis (2022)].
[74] Sarah Goldman, Anna Aspenson, Prashasti Bhatnagar and Robert Martin, Essential and in Crisis: A Review of the Public Health Threats Facing Farmworkers in the U.S., Center for a Livable Future (May 2021), https://bit.ly/3K213KU.
[75] Michelle Tigchelaar, David Battisti & June Spector, Work Adaptations Insufficient to Address Growing Heat Risk for U.S. Agricultural Workers, 15(9) Center Environmental Research Letters (Aug. 25, 2020), https://bit.ly/3z1vevP. For example, the average piece rate for tomato pickers in Florida is 50 cents for every 32-lbs of tomatoes picked. Farmworker Facts and Figures, Research Coalition of Immokalee Workers (accessed June 22, 2022), https://bit.ly/3CZMsME.
[76] Rising Temperatures Intensify Risks for Florida Farmworkers, The CLEO Institute (May 28, 2021), https://bit.ly/3FXCBIQ. Research has shown the odds of acute kidney injury to be dramatically increased in female agricultural workers paid on a piece rate basis. Moyce et al., Kidney Function in California Agricultural Workers (2017).
[77] Erik Hansson, Ali Mansourian, Mahdi Farnaghi, Max Petzold and Kristina Jakobsson, An Ecological Study of Chronic Kidney Disease in Five Mesoamerican Countries: Associations With Crop and Heat, 21 BMC Public Health Article number 840 (May 1, 2021), https://bit.ly/3mn1e9W; Richard J. Johnson, Catharina Wesseling and Lee S. Newman, Chronic Kidney Disease of Unknown Cause in Agricultural Communities, 380 New England Journal of Medicine 1843-1852 (May 19, 2019), https://bit.ly/3jPhq23.
[78] See, e.g., Jaime Butler-Dawson, Lyndsay Krisher, Miranda Dally, Katherine A. James, Richard J. Johnson, Diana Jaramillo, Hillary Yoder, Evan C. Johnson, Daniel Pilloni, Claudia Asensio, Alex Cruz and Lee S. Newman, Sugarcane Workweek Study: Risk Factors for Daily Changes in Creatinine, 6(9) Kidney International Reports 2404-2414 (Sep. 2021), https://bit.ly/3QIFenh; Christopher L. Chapman, Blair D. Johnson, Mark D. Parker, David Hostler, Riana R. Pryor and Zachary Schlader, Kidney Physiology and Pathophysiology During Heat Stress and the Modification by Exercise, Dehydration, Heat Acclimation and Aging, 8(2) Temperature: Multidisciplinary Biomedical Journal 108-159 (2021), https://bit.ly/3bqvYkj [hereinafter Chapman et al., Kidney Physiology and Pathophysiology During Heat Stress (2021)].
[79] Chapman et al., Kidney Physiology and Pathophysiology During Heat Stress (2021).
[80] Jacqueline Mix, Lisa Elon, Valerie Vi Thien Mac, Joan Flocks, Eugenia Economos, Antonio J. Tovar-Aguilar, Vicki Stover Hertzberg and Linda A. McCauley, Hydration Status, Kidney Function, and Kidney Injury in Florida Agricultural Workers, 60(5) Journal of Occupational and Environmental Medicine e253–60 (May 2018), https://bit.ly/3a2T2Ip.
[81] Id.
[82] El Khayat et al., Impacts of Climate Change and Heat Stress on Farmworkers’ Health: A Scoping Review (2022).
[83] Dong et al., Heat-related Death in Construction Workers (2019).
[84] Id.
[85] Id.
[86] Id.
[87] Id.
[88] See, e.g., Overview: Working in Outdoor and Indoor Heat Environments, OSHA (accessed on Oct 11, 2021), https://bit.ly/3oPDTiX.
[89] Documentation of the complaints was provided by Oregon OSHA in response to a FOIA request from HuffPost reporter Dave Jamieson, who generously shared them with Public Citizen.
[90] Umair Ifran, Extreme heat is killing American workers, The U.S. needs a national standard to protect workers from heat, Vox (July 21, 2021), https://bit.ly/3x5iZwE.
[91] California Firefighters Battle a Dozen Large Wildfires, AP News (August 23, 2021), https://bit.ly/3Mg0Nca.
[92] See, e.g., Paul J. Schramm, Ambarish Vaidyanathan, Lakshmi Radhakrishan, Abigail Gates, Kathleen Hartnett, Patrick Breysse, Heat-Related Emergency Department Visits During the Northwestern Heat Wave — United States, June 2021, 70(29) MMWR Morbidity and Mortality Weekly Report, Centers for Disease Control and Prevention 1020–1021 (July 23, 2021), https://bit.ly/3geBr04.
[93] Tord Kjellstrom, Bruno Lemke and Matthias Otto, Climate Conditions, Workplace Heat and Occupational Health in South-East Asia in the Context of Climate Change, 6(2) WHO South-East Asia Journal of Public Health 15-21 (Sep. 2017), https://bit.ly/3FN0jrq.
[94] Ioannou et al., Heat Strain Comprehensive Review and Meta-Analysis (2022).
[95] See, e.g., Fox 12 Staff, Local HVAC Companies Seeing Increase in Calls as Heat Wave Moves In, Fox 12 Oregon, (July 29, 2021), https://bit.ly/3ybC584; Kierra Elfalan, Air Conditioning Installers Slammed During Western Washington’s Heat Wave, King5 (June 28, 2021), https://bit.ly/3voVeAC.
[96] Nicholas K. Geranios and Andrew Selsky, Blackouts in U.S. Northwest Due to Heat Wave, Deaths Reported, AP News (June 29, 2021), https://bit.ly/3sz1ZzD.
[97] Aaron Gordon, The Heat Wave Is Literally Melting Portland’s Infrastructure, Vice (June 28, 2021), https://bit.ly/3yATasE.
[98] See, e.g., Workers’ Compensation Laws – State by State Comparison, National Federation of Independent Businesses (June17, 2017), https://bit.ly/3AWXiAN. Federal employees are covered by the Federal Employees’ Compensation Act. 51 U.S.C. §§8191 et seq. https://bit.ly/3C40H20.
[99] Workers’ Compensation, Farmworker Justice (accessed on June 22, 2022), https://bit.ly/3vuMkkY.
[100] NAWS 2022.
[101] See, e.g., What Employers Need To Know About Undocumented Workers Rights, 501(c) Agency Trust (May 5, 2021), https://bit.ly/2Z1bxHz; Undocumented Workers, Workplace Fairness (accessed on June 22, 2022), https://bit.ly/3lZ84lX; Workers’ Compensation, Farmworker Justice (accessed on June 22, 2022), https://bit.ly/3vuMkkY; Jeffrey Rhodes, Court Upholds Workers’ Comp Judgment for Undocumented Worker, SHRM (June 23, 2021), https://bit.ly/3GgPKNp.
[102] Texas Labor Code, Title 5 §§406.001 et seq. (2019), https://bit.ly/3C5CKaO. Texas does require construction companies on contract with the government to have workers’ compensation insurance coverage.
[103] Christopher J. Boggs, Employees Exempt from Workers’ Compensation, Insurance Journal (March 27, 2015), https://bit.ly/3yefmsf.
[104] See, e.g., Information Sheet, Employment Development Department, State of California, (accessed on June 22, 2022), https://bit.ly/2Z6BFRo.
[105] Employing Independent Contractors and Other Gig Workers, SHRM (July 9, 2021), https://bit.ly/3njvFwT.
[106] Fact Sheet 13: Employment Relationship Under the Fair Labor Standards Act (FLSA), Wage and Hour Division, Department of Labor (accessed on June 22, 2022), https://bit.ly/3E75HDY.
[107] Nik Theodore, Bethany Boggess, Jackie Cornejo and Emily Timm, Build A Better South, Workers Defense Project (2017), https://bit.ly/3pi7WQB.
[108] Fabiana B. Nerbass, Roberto Pecoits-Filho, William F. Clark, Jessica M. Sontrop, Christopher W. McIntyre and Louise Moist, Occupational Heat Stress and Kidney Health: From Farms to Factories, 2(6) Kidney International Reports 998-1008 (Nov. 2017), https://bit.ly/3IwNuTg.
[109] National Environmental Public Health Tracking, CDC (accessed on Jan. 24, 2022), https://bit.ly/32tdqPk. Following the 2021 Pacific Northwest heat wave, the British Columbia Coroner’s Service asked physicians to consult the Coroner’s Service prior to determining cause of death if heat could have been a contributing factor so that a proper assessment could be made. Vaughn Palmer, B.C. Coroner’s Service Has Asked Doctors Not to Issue Death Certificates in Heat-Related Cases, Vancouver Sun (July 12, 2021), https://bit.ly/3KGpr57.
[110] All health insurance rates identified in this report are based on data gathered prior to the COVID-19 pandemic and may not reflect the current extent of uninsured workers in these occupations. A study analyzing data from the U.S. Census Bureau’s Household Pulse Survey estimates that 2.7 million people in the U.S. lost their health insurance between April 23-July 21, 2020 due to lost coverage through an employer. The decrease in insurance coverage was concentrated in states without Medicaid expansion, as Medicaid expansion states saw employment-based health insurance plans replaced with Medicaid for many of the newly unemployed. Of note, the majority of non-expansion states are in the southern half of the country where occupational heat stress is particularly problematic for outdoor workers. M. Kate Bundorf, Sumedha Gupta and Christine Kim, Trends in U.S. Health Insurance Coverage During the COVID-19 Pandemic, 2(9) JAMA Health Forum e212487 (Sep. 3, 2021), https://bit.ly/2XIJ5Km.
[111] NAWS 2022. Only 26% of agricultural workers with health insurance reported that their employer provided the health insurance.
[112] Jacob Passy, Workers in This Field Are the Least Likely to Have Health Insurance, Market Watch (March 22, 2018), https://on.mktw.net/3ydD2gd.
[113] Id.
[114] Id.
[115] Id.
[116] Heat Injury and Illness Prevention in Outdoor and Indoor Work Settings, 86(205) Federal Register 59309 (Oct. 27, 2021), https://bit.ly/3dosuj7. Public Citizen and more than 100 allied organization and occupational heat experts filed petitions with OSHA for an occupational heat standard in 2011 and 2018, as well as a petition for an Emergency Temporary Standard in 2021. Petitions to OSHA for a Heat Standard, Public Citizen (accessed on Jun 2, 2022), https://bit.ly/3HHqu3G.
[117] Workplace Safety and Health: Multiple Challenges Lengthen OSHA’s Standard Setting, U.S. Government Accountability Office (April, 2012), https://bit.ly/3N8oHG3.
[118] Juley Fulcher, OSHA Fails to Protect Workers From Extreme Heat Hazards: OSHRA Decisions Demonstrate the Need for an OSHA Heat Stress Standard, Public Citizen (June 30, 2020), https://bit.ly/3tztdGO [hereinafter Fulcher, OSHRA Decisions Demonstrate the Need for an OSHA Heat Stress Standard (2020)]; Secretary of Labor v. A.H. Sturgill Roofing Inc., OSHRC Docket No. 13-0224 (Feb. 28, 2019), https://bit.ly/3HElNaW.
[119] 29 U.S.C. § 655(c).
[120] Or. Admin. Rule 437-002-0155, https://bit.ly/3QBrYRn; Or. Admin. Rule 437-004-1130, https://bit.ly/3Oe2esE (both effective July 8, 2021); Amendments to outdoor heat exposure rules under Washington Administrative Code Chapters 296-62 and 296-307 (effective July 13, 2021), https://bit.ly/3xjAdXf.
[121] Press Release, Oregon OSHA, Oregon OSHA Adopts Emergency Rule Bolstering Protections for Workers Against the Hazards of High and Extreme Heat (July 8, 2021), https://bit.ly/3eoJhUg.
[122] Id.
[123] Hal Bernton, Washington Releases New Heat Rules to Increase Protections for Outdoor Workers, The Seattle Times (July 9, 2021), https://bit.ly/3erBhl4.
[124] Eli Rosenberg and Abha Bhattarai, Biden Administration, Workers Grapple with Health Threats Posed By Climate Change and Heat, The Washington Post (July 19, 2021), https://wapo.st/3kzOH2B.
[125] Stillman, Jonathon, Heat Waves, The New Normal: Summertime Temperature Extremes Will Impact Animals, Ecosystems and Human Communities, 34 Physiology 86-100 (March 2019), https://bit.ly/2UUiwju.
[126] Kristina Dahl, Erika Spanberger-Siegfried, Rachel Licker, Astrid Caldas, Rachel Cleetus, Shana Uvardy, Juan Declet-Barreto, Pamela Worth, Killer Heat in the United States: Climate Choices and the Future of Dangerously Hot Days, Union of Concerned Scientists, 3 (July 2, 2019), http://bit.ly/3yCPuo1; E.M. Fischer, S. Sippel and R. Knutti, Increasing Probability of Record-Shattering Climate Extremes, 11 Nature Climate Change 689-695 (Aug. 2021), https://go.nature.com/3leXCXx.
[127] R. Jisung Park et al., Temperature, Workplace Safety, and Labor Market Inequality (2021), 5.
[128] Cal. Code. Regs., tit. 8, § 3395 , Heat Illness Prevention in Outdoor Places of Employment (enacted in 2005), http://bit.ly/3p0xOy7.
[129] Fulcher, OSHRA Decisions Demonstrate the Need for an OSHA Heat Stress Standard (2020).
[130] Secretary of Labor v. United States Postal Service, National Association of Letter Carriers (NALC) and National Rural Letter Carriers’ Association (NRLCA), OSHRC Docket Nos. 16-1713, https://bit.ly/3zY8EHX; 16-1813, https://bit.ly/39LQdf1; 16-1872, https://bit.ly/3NeBsyT; 17-0023, https://bit.ly/3bo2XJc; 17-0279, https://bit.ly/3xNO0Yf (July 15, 2020).
[131] Id.
[132] Id. These cases remain under review by OSHRC, and Public Citizen supports OSHA’s position in that matter.