The Cost of Inaction
The Failure of Employers to Mitigate the Effects of Heat Stress on Workers Causes Preventable Heat-related Illness, Injury and Fatalities and Costs the U.S. Economy $100 Billion Each Year.
By Juley Fulcher
Key Findings
- The cost of workplace heat stress in the U.S. based on lost work time due to reduced worker capacity is estimated to be nearly $100 billion every year.
- The physical and mental capacity of workers to function drops significantly as heat and humidity increase. For example, when it’s 86°F and the relative humidity is 45%, a worker can only function at 85% of their full capacity. When it’s 95°F with 75% humidity worker capacity drops below 50%.
- Productivity of workers declines approximately 2.6% per degree Celsius above a Wet Bulb Globe Temperature (WBGT) of 24°C (75.2°F). The WBGT is a measure that combines temperature, relative humidity, radiant heat sources (like direct sunlight or heat-generating machinery) and wind speed.
- The dangers of occupational heat stress are overwhelmingly borne by low-income workers, with the lowest-paid 20% of workers suffering five times as many heat-related injuries as the highest-paid 20%.
- Research has shown that medical costs increase 41.6% per degree Celsius when the temperature exceeds 33°C (91.4°F).
- There are many ways employers can mitigate heat stress in the workplace like—access to cool drinking water and adequate “cool down” breaks in a shaded or air-conditioned space.
- It is essential that OSHA issue an interim OSHA rule to prevent heat-related illness, injury and death in indoor and outdoor workers, both to protect workers and to reduce the clear burden on the economy.
Introduction
Every year in the United States as many as 2,000 workers lose their lives to excessive heat in the workplace[1] — a price no worker should ever have to pay. The impact of these lost lives on their families and loved ones is immeasurable. Up to 170,000 additional workers are injured in heat stress related accidents on the job,[2] potentially resulting in long-term disabilities that can not only diminish worker income, but also have detrimental effects on worker health and reduce quality of life.
The Occupational Health and Safety Administration (OSHA) is in the process of developing a heat standard requiring employers to protect workers from excessive heat exposure in the workplace. The process involves weighing the input of all stakeholders — workers, worker advocates, unions, heat-stress experts, industry representatives, employers, and the public. On average, it takes OSHA seven to eight years to complete a standard.[3] A required element of the process is estimating the financial costs to employers of implementing various proposed requirements and conducting a cost-benefit analysis.[4]
Because it’s impossible to put a real price on lost lives, human suffering or the workers’ fears that they may not return home due to injury, there is no acceptable cost-benefit analysis to determine whether employers should implement basic protocols that protect workers from heat-related illness, injury, and death. Nor should there be.
Though it’s not possible to weigh lives against costs, it is important to understand the cost of inaction and delay.
This report addresses the substantial financial costs of failing to protect workers from heat stress. It discusses the human and economic costs of workplace heat stress for employees. The report outlines the myriad financial costs to employers who do not implement simple protocols to mitigate heat stress on the job, with a focus on the reduced physical and mental capacity of their employees when working in hot and humid conditions.
Each year employers and workers are paying a heavy price for unmitigated workplace heat stress and the toll on the economy is immense. And each year without an OSHA heat stress standard puts the health and lives of more workers on the line. OSHA must issue an interim heat standard to protect workers while a final rule is promulgated.
Background
Heat stress is a function of internally generated heat — metabolic heat, external environmental heat and other factors that reduce the effectiveness of our natural bodily cooling systems. Metabolic heat increases as workload increases. Sweat is produced so that the process of evaporation can release body heat and blood is pumped to the surface of the skin to be cooled by the surrounding air. However, high humidity reduces the evaporation of sweat and high environmental temperatures introduce more heat into the blood at the surface of the skin.
The bodily response is more sweating and more blood sent to the surface of the skin. But, as more blood is diverted to the skin, less blood is being directed to the muscles and the brain.[5] Without replenishment, excessive sweating causes dehydration, thickening the blood and making the heart work harder. A greater proportion of the cardiac output is devoted to cooling the body and the proportion available for physical and mental work decreases.[6] As the body’s cooling systems strain to keep the body cool, heat-related illness can occur.
Heat-related illnesses range in severity from mild heat rash to more severe illnesses such as rhabdomyolysis, acute kidney injury, heat stroke and heat-stress induced cardiac arrest. Workers who survive these more severe heat-related illnesses are often burdened with long term health effects, including muscle damage, organ damage and chronic kidney disease. Excessive heat in the workplace can also exacerbate existing chronic conditions like diabetes, COPD and cardiac disease, complicating the health care of these workers and potentially shaving years off their lives.
The systems of heat-related illnesses include heavy sweating, fatigue, nausea, headache, loss of balance and cognitive function, fainting, muscle cramps, and more. These symptoms can easily lead to accidents with a range of consequences to one or more people, including injuries, long-term disabilities or even fatalities.
There are several ways employers can mitigate heat stress in the workplace. The simplest of these is providing workers with consistent access to cool drinking water and adequate “cool down” breaks in a shaded or air-conditioned space. Employers can make a variety of simple alterations such as heat shields for workers stationed next to heat-generating machinery or awnings over windows to block the sunlight. Employers can also increase ventilation or air conditioning in workspaces. While these alterations may involve more up-front costs, they are the most effective in reducing the impact on heat stress.
The Cost to Workers
Workers and their families can face serious financial hardships as a result of heat-related illness or injury on the job.
More than 60% of workers in the U.S. live paycheck-to-paycheck.[7] That number rises to 78% for workers who make less than $50,000 per year.[8] And of those living paycheck-to-paycheck, an estimated 21% adults are losing the battle — struggling to stretch those paychecks to cover their monthly bills.[9]
The dangers of occupational heat stress are overwhelmingly borne by low-income workers, with the lowest-paid 20% of workers suffering five times as many heat-related injuries as the highest-paid 20%.[10] Struggling to make ends meet, these workers can’t afford to lose income. For many hourly, piece-rate and contract workers, even a couple days of missed work can put food and housing security at risk.
When coupled with the underlying health of the individual, the time needed to recover could be days, weeks or even months. As the days needed for recovery mount, workers are more likely to lose their jobs.
Even when workers that have recovered from heat related injuries are able to work again, they may be unable to do the same tasks or handle a full workload. While the employer may be able to change the employee’s duties on a temporary or permanent basis, many employers are unable or unwilling to make such an accommodation. New or exacerbated chronic conditions and long-term or permanent injuries may make it impossible for the worker to return to the same type of work, adding the cost of retraining for a different career.
Lost jobs and worker disability are a major cause of financial distress.[11] More than a third of low-wage workers would not be able to cover one month of living expenses, including basic necessities like food, if they lost their income.[12] And 16% of low-wage workers would not be able to cover their basic costs for a week if they lost their income.[13] Thirty-eight percent of white workers making less than $50,000 a year could pay for a financial setback of $400.[14] Sadly, that percentage increases to 53% of Black workers and 48% of Latino workers.[15]
With lost income and overdue bills, workers and their families may be evicted from rental housing or their home may go into foreclosure.[16] A minimum wage worker needs to work two full-time jobs to rent a one-bedroom home.[17 Evictions and foreclosures are on the rise.[18] As of August, 2022, more than 20 million households in the U.S. have been unable to keep up with their utility bills.[19] Many turn to credit cards to pay for essentials,[20] then are unable to pay the monthly credit card bills. Unpaid bills may go into collections. The worker may have to declare bankruptcy. In fact, medical bills are the leading cause of bankruptcy.[21] The consequences can mean a destroyed credit rating that prohibits recovery. Families who lose a loved one to workplace heat stress may suffer these same consequences while enduring immeasurable personal loss.
Healthcare is a significant financial burden for workers who experience heat-related illness or injury. Even heat-related fatalities can leave families with an exorbitant bill for emergency health services performed before a worker’s tragic passing.
In a study of treatment of Army personnel for heat illness, the average price tag was $599, but costs climbed as high $4,094 for inpatient care for heat exhaustion and $7,453 for inpatient care following a heat stroke.[22] Researchers of heat-related illness, specifically heat exhaustion and heat stroke, in Army Ranger trainees estimated that the cost for outpatient treatment for heat exhaustion ranged from $3,024 to $4,327, while the cost of an inpatient treatment for heat stroke ranged from $5,000 to $6,878.[23]
In a system without universal health care, like the U.S., individuals have to pay for essential health services. In theory when a worker has suffered a heat-related illness or injury on the job, those bills are paid by workers’ compensation insurance and health insurance. But in reality, the cost of health care to address heat illness and injuries often comes directly from the pockets of workers.
States have different rules about when employers are required to have workers’ compensation insurance and which workers it must cover.[24] These rules often leave the workers that are most susceptible to heat-related illness, injury and death without access to workers’ compensation benefits. For example, employers are exempt from providing workers’ compensation for farmworkers in 16 states.[25] In most states, independent contractors, day laborers and/or temporary employees, roles commonly seen in construction and seasonal outdoor employment, receive no workers’ compensation benefits from the employer who hired them.[26] Texas doesn’t require non-governmental employers to have workers’ compensation insurance at all.[27]
Many of those with high heat hazard jobs lack access to affordable health insurance. In fact, the 20 occupations in the U.S. least likely to have health insurance are all jobs likely to put workers in danger of heat stress, including roofers, cement and brick masons, farmworkers, cooks, dishwashers, and grounds maintenance workers.[28] Even those with health insurance struggle with the cost of healthcare. More than a third of low-wage workers who have health insurance through their employers report skipping medication or doctor visits in the past year.[29] This is mostly because workers can‘t afford the copay or deductible or they could not get time off from work to go to the doctor.[30]
The Cost to Employers
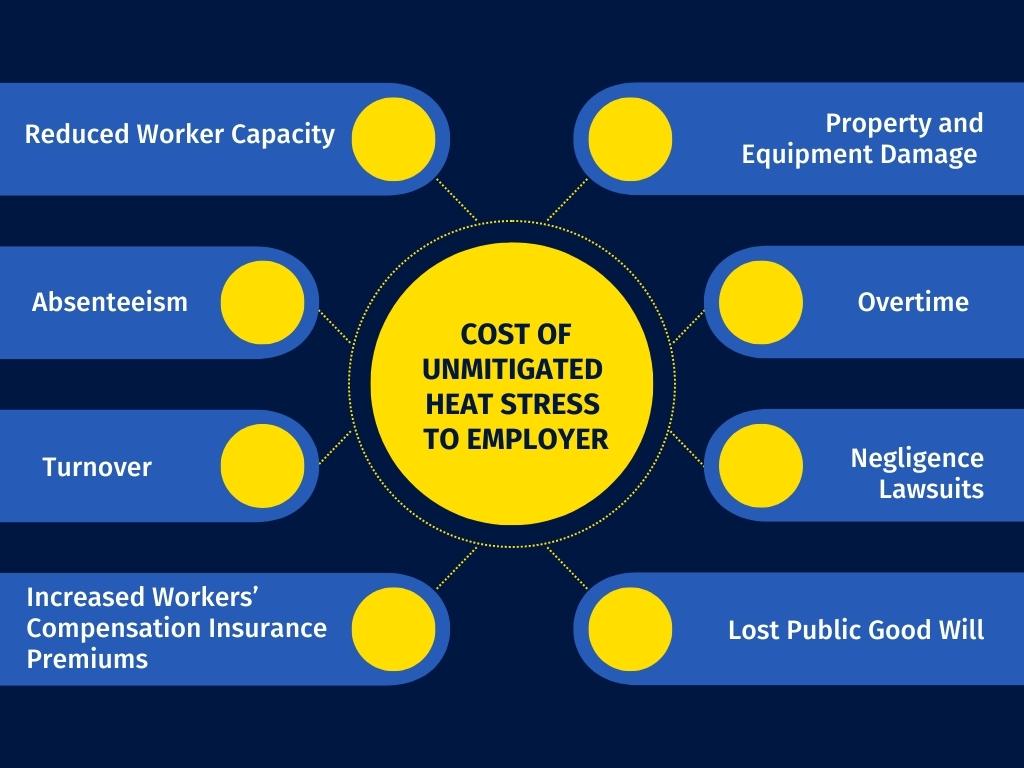
Failing to mitigate workplace heat hazards leaves employers financially burdened in multiple ways. Employers face reduced productivity resulting from absenteeism and turnover when workers experience heat-related illness or injury, as well as general reduced worker capacity because of heat stress. Employers may have to pay for overtime to replace absent workers. They may be straddled with the cost to repair or replace damaged equipment, vehicles and property owing to accidents caused by heat stress. Workers’ compensation premiums may increase due to the number of claims by injured workers. By not addressing an obvious risk of worker heat-related illness or injury, an employer may be sued for negligence and forced to pay court judgements and associated legal fees. A reputation as an unsafe workplace also means the potential loss of the public good will and, with it, customers. The OSHA $afety Pays tool estimates the average direct costs of a single “heat prostration” injury in the workplace to be $37,658 with an estimated indirect cost of $41,423.[31] It also estimates average syncope (fainting) direct costs at more than $30,000 and indirect costs exceeding $33,000.[32] In general, heat stress prevention is cheaper than responding to the consequences of a tragedy.
Worker Capacity
Employers sometimes raise concerns about the cost of lost productivity when providing breaks to workers. However, heat stress reduces the physical and mental capacity for work. Without heat stress mitigation, such as opportunities to rest in a cool area and drink water, heat stress continues to increase and worker capacity decreases, ultimately reaching a point when work is no longer physically possible.
As noted above, the strain to keep the body cool, causes fatigue, deficits in motor and cognitive function, dizziness, nausea, and other symptoms of heat-related illness that become increasingly severe. Even the earliest symptoms of heat stress limit the ability to function, interfering with worker effectiveness and increasing the risk of mistakes, accidents and injuries.
Periodically stopping physical exertion helps diminish heat generated by the body, allowing heat dissipation to exceed heat production. When coupled with conditions or practices that accelerate dissipation, such as a “cool down” environment or drinking cool water, it can be even more effective. But when employers fail to give workers adequate time to rest and cool down, productivity can be drastically decreased by the limitations in worker capacity.
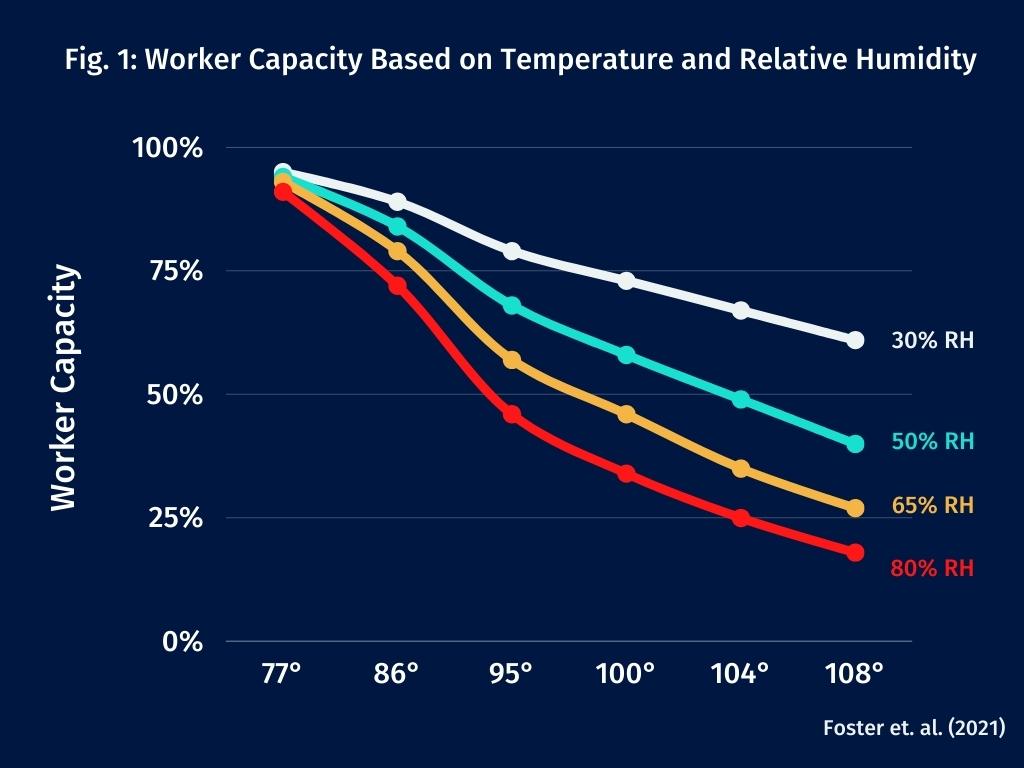
In the losing battle against high surrounding temperatures, one of the body’s natural survival mechanisms is to slow the pace of work. Allowing workers to self-pace is one of the most impactful mitigation strategies to reduce heat-related illness, injury or death.[33] Employers who use quota systems and piece-rate pay remove that option for employees, forcing workers to maintain the same pace as temperatures rise , increasing the heat stress danger to workers.But worker self-pacing alone is not enough. Even when workers are able to slow the pace of work, metabolic heat production can outpace cooling in a hot environment. Numerous studies of worker productivity demonstrate the reduction in worker capacity with heat stress. Foster et al. developed a model to predict the reduction in work capacity associated with increases in ambient temperature and relative humidity (see Figure 1).[34] For example, a worker is able to work at 95% of full capacity when it’s 77° with a relative humidity of 30%.[35] However, worker capacity drops to 68% when it’s 95° with a relative humidity of 50%. And worker capacity drops to 25% when it’s 104° with a relative humidity of 80%.[36] This is the equivalent of only working 15 minutes each hour.
The Foster et al. model shows the dramatic impact temperature and humidity can have on worker capacity. However, it is likely a conservative estimate. The temperature in the Foster et al. study used the standard measure of ambient temperature — temperature in the shade. It doesn’t include the impact of solar radiation for those working outside in the sun, a significant factor in causing heat stress. Another study used the Wet Bulb Globe Temperature (WBGT), which combines temperature, humidity, radiant heat (the sun, heat-generating machinery) and wind speed, found that worker productive loss in the shade was 80% lower than productivity loss of those working in the sun.[37] In other words, working in the sun decreases worker capacity well beyond the predictions in the Foster et al. model.
A meta-analysis of 7 studies in multiple countries found that worker productivity declines averaged 2.6% per degree Celsius above a Wet Bulb Globe Temperature (WBGT)[38] of 24°C (75.2°F).[39] And workers are aware of their lost productivity when they workin the heat. For example, A study of indoor and outdoor workers in Australia found that 93% of workers who experienced heat stress on the job self-reported lower productivity. These workers reported being 35% less productive when experiencing heat stress.[40] Annually, this totaled 27.1 hours lost productivity per worker.[41]

Lowered worker capacity also means increased workplace injuries. A meta-analysis of 17 studies worldwide also showed an average 1% increase in occupational injuries for every 1 degree C above 20.9°C (69.6° F). Increases were highest, up to 1.7% increase in injuries per 1 degree C, in humid subtropical climates, such as the southeastern parts of the U.S.[42] A study of agricultural workers in Washington State found the odds of traumatic injuries in cherry harvesters, primarily from ladder falls, increased 1.53% for every 1 degree C above 25°C (77° F).[43]
Ultimately, failing to provide adequate “cool down” breaks to employees and the resulting declines in worker capacity come with a sizable price tag for employers. It is compounded by absenteeism and turnover caused by heat-related injuries precipitated by reduced worker capacity, as well as increased heat-related illnesses. These, in turn, cascade into a wide array of financial costs can even result in the loss of consumer support.
The Cost to the Economy
It is estimated that the annual global cost of lost work time due to reduced worker capacity is $2.1 trillion.[44] The U.S. alone is losing more than $98 billion every year.[45] More than 40% of the global cost is currently borne by India and China,[46] countries that are four times the size of the U.S.[47] In 87 countries, humid heat contributed to an annual labor capacity loss in outdoor workers equal to four weeks or more per person.[48]
The cost of lowered work capacity has an outsized impact on many countries in Asia and Africa that are on the front lines of climate change, with those in South Asia, Sub-Saharan Africa, the Middle East and North Africa expected to see the largest drops in GDP due to increasing heat and heat waves in the next 30 years.[49] The dramatically increasing heat and humidity has caused particularly heavy drops in GDP in Indonesia, Saudi Arabia, Sudan, Nigeria, Thailand, Pakistan and the Philippines.[50] Global costs are expected to continue to rise with estimates of as much as $2.4 trillion in lost productivity due to heat-induced decreases in worker capacity by 2030,[51] a figure that could be greatly curtailed if employers implement simple heat stress mitigation strategies.
Heat-related injuries in California are estimated to have a social cost between $525 million and $875 million annually.[52] And a U.S. military report estimated that heat stroke and heat exhaustion cost the U.S. Army $350,000 in lost duty days and $36 million in indirect costs between 2016 and 2018.[53]
In the United States, 62% of all counties annually lose more than 0.5% of gross value added (GVA) due to heat-related worker productivity losses.[54] The GVA is a productivity measure reflecting the value of goods and services produced in the area, industry or sector derived as the output minus immediate consumption. Productivity losses are greater than $5 million per year in approximately the same percentage of counties.[55] Texas counties lose a combined $30 billion in a typical year, the equivalent of about 1.5% of GVA, and Florida loses $11 billion per year.[56] It is no surprise that, by proportion, the productivity losses are greatest in agriculture and construction.[57] Because many indoor businesses lack air conditioning or adequate ventilation, the services sector loses about $600 million annually, the largest overall cost.[58] This includes restaurants, transportation, hospitality, and warehousing.[59]
Research on the economic costs of occupational heat stress in other countries also reveal a stark reality in those nations as well. For example, the combined costs of absenteeism and reduced worker capacity due to heat stress causes annual estimated loss of US $6.2 billion in labor productivity for the Australian economy due to heat stress.[60]
In Spain an analysis of 16 million workers compensation claims between 1994 and 2013, showed an estimated annual economic burden of occupational heat-related injuries coming in at €319.4 million (319.8 million in current U.S. dollars).[61] This includes the cost of an estimated 580,000 days of work lost every year due to high heat in Spain, a country of 46.5 million people.[62] The total annual price tag was broken down into four categories.
- Business productivity — The cost of maintaining the same level of production when workers are out on sick leave due to heat illness/injury, such as overtime for other workers and money used for substitution and training, is estimated to be €59.2 million ($59.3 million) annually.
- Worker income loss — The total income lost when workers are unable to return to work after the heat-related illness or injury is estimated to be €49.2 million ($49.3 million) per year.
- Disability pain and suffering — The cost of pain and suffering associated with the workers’ level of disability is €183 million ($183.2 million) annually.
- Health care — The estimated health care cost is €28 million ($28 million) every year due to high heat.[63]
Health Care Costs
Healthcare costs for heat-related illness and injury also have a dramatic effect on the economy. While many costs fall on the shoulders of the injured workers, health insurance, workers’ compensation and Medicaid are other major sources of cost coverage for workers injured by heat on the job. In turn, health insurance premiums rise for everyone and more tax dollars are needed to fund Medicaid.
Between 2016-2018, heat exhaustion and heat stroke in soldiers cost the U.S. Army $7.3 million in direct health care costs.[64] Though data on the impact of health care for occupational heat-related illnesses and injuries on the U.S. economy in the United States is limited, data from other nations is instructive. A study of workers’ compensation claims for heat stress illness (not including heat stress injuries) in South Australia between 2000-2014 found a total of more than AU$6 million in annual medical costs, approximately US$4 million.[65] The research showed that medical costs increased 41.6% per degree Celsius when the temperature exceeded 33°C (91.4°F).[66]
For comparison, South Australia has a population of 1.77 million people while the U.S. has a population of 332 million, 188 times more people. And we pay more than double the price per person for health care than Australia.[67] A basic extrapolation hints at a U.S. health care cost for occupational heat stress upwards of a billion dollars every year.[68] A similar extrapolation of the health care cost of occupational injuries due to high heat in Spain, as indicated above, would put the price tag for the U.S. closer to $600 million per year.[69] Certainly, these cost estimates for the United States have limited validity, but the economic research from both countries point to a likely very substantial sticker price for health care for heat-related illness and injuries on the job in the U.S.
Occupational heat stress is a drag on the national and world economy. As extraordinary heat waves are increasing around the globe, a growing number of nations are focusing on how to protect workers.[70] With an eye toward the rapidly growing costs of heat stress in the workplace, it is essential for OSHA to put an effective heat standard in place without delay.
Conclusion
The burden of occupational heat stress on the economy is tremendous and rapidly growing. Failing to mitigate the hazard for workers has great financial consequences for employers. And the price paid by workers is incalculable and unacceptable, not only in dollars, but more importantly in the loss of health, safety and life.
As we consider all of these costs, the question is not whether we can afford to protect workers from the impact of heat stress. It’s whether we can afford not to.
[1] Juley Fulcher, Boiling Point: OSHA Must Act Immediately to Protect Workers from Deadly Temperatures, Public Citizen (June 2022), https://www.citizen.org/article/boiling-point/ [hereinafter Fulcher, Boiling Point (June, 2022)].
[2] Id.
[3] Workplace Safety and Health: Multiple Challenges Lengthen OSHA’s Standard Setting, U.S. Government Accountability Office (April, 2012), https://bit.ly/3N8oHG3.
[4] See, e.g., Congressional Research Service, Cost-Benefit Analysis in Federal Agency Rulemaking (March 8, 2022), https://bit.ly/3RrAOjG.
[5] Josh Foster, James W. Smallcombe, Simon Hodder, Ollie Jay, Andreas D. Flouris, Lars Nybo and George Havenith, An Advanced Empirical Model for Quantifying the Impact of Heat and Climate Change on Human Physical Work Capacity, 65 International Journal of Biometeorology 1‐15 (2021), https://bit.ly/3xT1FhG [hereinafter Foster et al., Quantifying Impact of Heat on Work Capacity (2021)]; Margaret C. Morrissey, Gabrielle J. Brewer, Tyler Quinn and Douglas J. Casa, Impact of Occupational Heat Stress on Worker Productivity and Economic Cost, American Journal of Industrial Medicine (Sep. 2021), https://bit.ly/3RdM2YQ.
[6] Foster et al., Quantifying Impact of Heat on Work Capacity (2021).
[7] PYMNTS.com and Lending Club, New Reality Check: The Paycheck-to-Paycheck Report (Aug 2022), https://bit.ly/3dGfdq2.
[8] Id.
[9] Id.
[10] R. Jisung Park, Nora Pankratz & A. Patrick Behrer, Temperature, Workplace Safety, and Labor Market Inequality, IZA Institute of Labor Economics DP No. 14560 3 (July 2021), https://bit.ly/2V3WriI [hereinafter R. Jisung Park et al., Temperature, Workplace Safety, and Labor Market Inequality (2021)].
[11] PYMNTS.com and Lending Club, New Reality Check: The Paycheck-to-Paycheck Report (June/July 2022), https://bit.ly/3C9e57G.
[12] Beth Brockland and Tanya Ladha, Financial Health of Workers in Low-wage Jobs, Financial Health Network (July 28, 2022), https://bit.ly/3r98fNf [hereinafter Brockland and Ladha, Financial Health of Workers in Low-wage Jobs (2022)].
[13] Id.
[14] Economic Well-Being of U.S.Households in 2021, Board of Governors of the Federal Reserve Systems (May, 2022), https://bit.ly/3RjmV75.
[15] Id.
[16] National Low Income Housing Coalition, Out of Reach: The High Cost of Housing (2022), https://bit.ly/3BRIgz0.
[17] Id.
[18] National Low Income Housing Coalition, Out of Reach: The High Cost of Housing (2022), https://bit.ly/3brigz0; Alisa Wolfman, Foreclosures are on the Rise. Here’s What That Says About the Housing Market, Market Watch (March 19, 2022), https://on.mktw.net/3dwdbge.
[19] Will Wade and Mark Chediak, A ‘Tsunami of Shutoffs’: 20 Million US Homes Are Behind on Energy Bills, Bloomberg: Business Week (Aug 23, 2022), https://bloom.bg/3DTitc4.
[20] Adam Hardy, 40% of Americans are Struggling to Pay Their Bills Right Now, Money (July 22, 2022), https://bit.ly/3xU7xHm.
[21] Brockland and Ladha, Financial Health of Workers in Low-wage Jobs (2022).
[22] Lanna Forrest, Alexis Maule, Ashleigh McCabe, Julianna Kebisek, Ryan Steelman & John Ambrose, Brief Report: Direct Care Cost of Heat Illness to the Army, 2016-2018, Health.Mil (June 1, 2020), https://bit.ly/37UQFTp
[hereinafter Forrest et al. Direct Care Cost of Heat Illness to the Army ( 2020)].
[23] David DeGroot, Robert W. Kenefick and Michael Sawka, Impact of arm immersion cooling during Ranger training on exertional heat illness and treatment costs, 108(11) Military Medicine 1178-1183 (2015), https://bit.ly/3DTZnCT. Of note, the study showed that immediate immersion of the arm in cold ice water can reduce the severity of the heat illness experienced. Compared to cases where arm immersion cooling was not used, the implementation of arm immersion cooling protocols increased the proportion of heat illness sufferers able to be treated at the Ranger Aid Station and released by approximately 3.8-fold, while the proportion who had to be transported to a hospital for medical care and/or admitted to the hospital were each reduced approximately 40%.
[24] See, e.g., Workers’ Compensation Laws – State by State Comparison, National Federation of Independent Businesses (June17, 2017), https://bit.ly/3AWXiAN. Federal employees are covered by the Federal Employees’ Compensation Act. 51 U.S.C. §§8191 et seq. https://bit.ly/3C40H20.
[25] Workers’ Compensation, Farmworker Justice (accessed on June 22, 2022), https://bit.ly/3vuMkkY.
[26] Christopher J. Boggs, Employees Exempt from Workers’ Compensation, Insurance Journal (March 27, 2015), https://bit.ly/3yefmsf.
[27] Texas Labor Code, Title 5 §§406.001 et seq. (2019), https://bit.ly/3C5CKaO. Texas does require construction companies on contract with the government to have workers’ compensation insurance coverage.
[28] See Fulcher, Boiling Point (June 2022). Health insurance rates identified in this report are based on data gathered prior to the COVID-19 pandemic and may not reflect the current extent of uninsured workers in these occupations. A study analyzing data from the U.S. Census Bureau’s Household Pulse Survey estimates that 2.7 million people in the U.S. lost their health insurance between April 23-July 21, 2020 due to lost coverage through an employer. The decrease in insurance coverage was concentrated in states without Medicaid expansion, as Medicaid expansion states saw employment-based health insurance plans replaced with Medicaid for many of the newly unemployed. Of note, the majority of non-expansion states are in the southern half of the country where occupational heat stress is particularly problematic for outdoor workers. M. Kate Bundorf, Sumedha Gupta and Christine Kim, Trends in U.S. Health Insurance Coverage During the COVID-19 Pandemic, 2(9) JAMA Health Forum e212487 (Sep. 3, 2021), https://bit.ly/2XIJ5Km.
[29] Brockland and Ladha, Financial Health of Workers in Low-wage Jobs (2022).
[30] Id.
[31] OSHA’s $afety Pays, OSHA (accessed on Sep. 26, 2022), https://bit.ly/3xRlZQE.
[32] Id.
[33] Leonidas G. Ioannou, Konstantinos Mantzios, Lydia Tsoutsoubi, Eleni Nintou, Maria Vliora , Paraskevi Gkiata, Constantinos N. Dallas, Giorgos Gkikas, Gerasimos Agaliotis, Kostas Sfakianakis, Areti K. Kapnia, Davide J. Testa, Tânia Amorim, Petros C. Dinas, Tiago S. Mayor, Chuansi Gao, Lars Nybo and Andreas D. Flouris , Occupational Heat Stress: Multi-Country Observations and Interventions, 18 International Journal of Environmental Research and Public Health 6303 (June 10, 2021), https://bit.ly/3kdZbUr.
[34] Foster et al., Quantifying Impact of Heat on Work Capacity (2021).
[35] Id. Research has shown that the optimal work environment for 100% productivity is between 59°F and 65%F.
[36] Id.
[37] Marco Morabito, Alessandro Messeri, Alfonso Crisci, Junzhe Bao, Rui Ma, Simone Orlandini, Cunrui Huang and Tord Kjellstrom, Heat-Related Productivity Loss: Benefits Derived by Working in the Shade or Work-Time Shifting, 70(3) International Journal of Productivity and Performance Management 507-525 (2021), https://bit.ly/3UE7A3P.
[38] The Wet Bulb Globe Temperature (WBGT) measures heat impact on the body by combining ambient temperature, relative humidity, air movement (wind speed) and solar radiant heat (e.g., heat-generated machinery, sunlight angle and cloud cover). It is a more accurate measure for calculating workplace heat stress than than the heat index. The heat index is a measure of apparent heat in the shade and as much as 15°F must be added to the heat index to get a measure of heat impact on the body in direct sunlight.
[39] Andreas D. Flouris, Petros C. Dinas, Leonidas G. Ioannou, Lars Nybo, George Havenith, Glen P. Kenny and Tord Kjellstrom, Workers’ Health and Productivity Under Occupational Heat Strain: Systematic Review and Meta-Analysis, 2(12) The Lancet Planetary Health E521-E531 (Dec. 1, 2018), https://bit.ly/3DRPl2z.
[40] Kerstin K. Zander, Wouter J. W. Botzen, Elspeth Oppermann, Tord Kjellstrom and Stephen T. Garnett, Heat Stress Causes Substantial Labour Productivity Loss in Australia, 5 Nature Climate Change 647, 648 (July 2015), https://bit.ly/3lx2YvI [hereinafter Zander et al. Heat Stress Causes Substantial Labour Productivity Loss in Australia (2015)].
[41] Id.
[42] Syeda Hira Fatima, Paul Rothmore, Lynne C. Giles, Blesson M. Varghese and Peng Bi, Extreme Heat and Occupational Injuries in Different Climate Zones: A Systematic Review and Meta-analysis of Epidemiological Evidence, 148 Environment International 106384 (March, 2021), https://bit.ly/3jGUEcL.
[43] June T. Spector, David K. Bonauto, Lianne Sheppard, Tania Busch-Isaksen, Miriam Calkins, Darrin Adams, Max Lieblich and Richard A. Fenske, A Case-crossover Study of Heat Exposure and Injury Risk in Outdoor Agricultural Workers, Plos One (Oct. 7, 2016), https://bit.ly/2ZQLxiz.
[44] Luke A. Parsons, Yuta J. Masuda, Timm Kroeger, Drew Shindell, Nicholas H. Wolff and June T. Spector, Global Labor Loss Due to Humid Heat Exposure Underestimated for Outdoor Workers, 17(1) Environmental Research Letters 014050 (2022), https://bit.ly/3DXvrWn [hereinafter Parsons et al., Global Labor Loss Due to Heat Exposure (2022)]. Purchasing Power Parity dollars (PPP$) is a measure to compare prices of goods between countries. In this study, the 2017 cost of lost labor due to the limits in worker capacity resulting from measures of heat and humidity was estimated for each country in their local currency. Each estimate was divided by the country’s GDP 2017 PPP conversion rate to U.S. dollars as determined by the World Bank .The sum of each national estimate is the global estimate of lost labor due to the limits in worker capacity resulting from measures of heat and humidity.
[45] Parsons et al., Global Labor Loss Due to Heat Exposure (2022).
[46] Id.
[47] U.S. Census Bureau Population Clock, U.S. Census Bureau (Oct. 3, 2022), https://bit.ly/3SWuPVn.
[48] Parsons et al., Global Labor Loss Due to Heat Exposure (2022). The 10 countries with the highest per capita loss in productivity among outdoor workers are Cambodia, Tuvalu, Brunei, Nauru, Micronesia, Palau, Sri Lanka, Ghana, Singapore and Thailand.
[49] Marc Jones, How Hard Could Climate Change Hit the Global Economy, and Where Would Suffer Most?, World Economic Forum (Apr. 29, 2022), https://bit.ly/3e2NG24.
[50] Parsons et al., Global Labor Loss Due to Heat Exposure (2022).
[51] Matthew A. Borg, Jianjun Xiang, Olga Anikeeva, Dino Pisaniello, Alana Hansen, Kerstin Zander, Keith Dear, Malcolm R. Sim and Peng Bi, Occupational Heat Stress and Economic Burden: A Review of Global Evidence, 195 Environmental Research 110781 (Apr. 2021), https://bit.ly/3l4z3Mf.
[52] R. Jisung Park et al., Temperature, Workplace Safety, and Labor Market Inequality, 29.
[53] Forrest et al. Direct Care Cost of Heat Illness to the Army ( 2020).
[54] Atlantic Council: Adrienne Arsht Rockefeller Foundation Resilience Center and Vivid Economics, Extreme Heat: The Economic and Social Consequences for the United States (August, 2021), https://bit.ly/3D8FGDA
[hereinafter Atlantic Council (2021)]. Only a handful of Alaskan counties currently have no economic losses.
[55] Id.
[56] Id.
[57] Id.
[58] Id.
[59] Id.
[60] Zander et al. Heat Stress Causes Substantial Labour Productivity Loss in Australia (2015).
[61] Èrica Martínez-Solanas, María López-Ruiz, Gregory A. Wellenius, Antonio Gasparrini, Jordi Sunyer, Fernando G. Benavides and Xavier Basagaña, Evaluation of the Impact of Ambient Temperatures on Occupational Injuries in Spain, 126(6) Environmental Health Perspectives (June 2018), https://bit.ly/3A9s7SC [hereinafter Martínez-Solanas et al., Occupational Injuries in Spain (2018).]. All rates calculated in this report use Foreign Exchange Rates (H.10/G.5), Board of Governors of the Federal Reserve System (Sep. 19, 2022), https://bit.ly/2Ylp50A.
[62] Martínez-Solanas et al., Occupational Injuries in Spain (2018).
[63] Id.
[64] Forrest et al. Direct Care Cost of Heat Illness to the Army ( 2020).
[65] Xianjun Xiang, Alana Hansen, Dino Pisaniello, Kieth Dear and Peng Bi, Correlates of Occupational Heat-Induced Illness Costs: Case Study of South Australia 2000 to 2014, 60(9) Journal of Occupational and Environmental Medicine e463-e469 (Sep, 2018), https://bit.ly/3l2Ek7c.
[66] Id.
[67] Based on data drawn from the Organisation for Economic Co-operation and Development (OECD) indicating the the cost of annual healthcare per capita in the U.S. in 2019 was $10,949, 2.23 times the cost in Australia of $4,919. OECD Statistics 2021, Organisation for Economic Co-operation and Development (data extracted on Oct. 24, 2021), https://bit.ly/3m7OqnI.
[68] $4.45 million (estimated annual cost) x 2.23 (healthcare cost adjustment) = $9,923,500 x 188 (population adjustment) = $1,865,618,000.
[69] The U.S. has a population 7.14 times greater than Spain, 332 million divided by 46.5 million. The annual cost of healthcare per capita in the U.S. in 2019 was $10,949 compared to $3,600 in Spain, more than 3 times larger. OECD Statistics 2021, Organisation for Economic Co-operation and Development (data extracted on Oct. 24, 2021), https://bit.ly/3m7OqnI. $28 million (estimated annual cost) x 3.04 (healthcare cost adjustment) = $85,120,000 x 7.14 (population adjustment) = $607,756,800.
[70] See, e.g., HEAT-SHIELD, Work-heat Action Plan (2020), https://bit.ly/3LIOju4.