Economic and Racial Inequality Are Intensifying the Killing Power of COVID-19 in the U.S.
Health Letter, August 2020
By Michael T. Abrams, M.P.H., Ph.D.
During the first six months of the COVID-19 pandemic in the U.S., 140,000 have died, nearly 60 million have filed for unemployment benefits and more than 25 million are without health care insurance. This is today in the United States of America, the wealthiest country in the world.
Additionally, there have been emotional protests in almost every major U.S. city in response to yet another white-on-black killing at the hands of law enforcement, as well as loads of inflammatory rhetoric and action from a president whose incompetence is matched only by his depravity. This violence, discord and unrest is extraordinary, yet also predictable.
Protesters and all citizens are being exhorted by leaders across the political spectrum to remain peaceful and physically distant, to slow the resurging spread of a highly infectious and dangerous virus for which there is no cure. But the pressures many Americans are feeling now run distinctively counter to the promises of their society. Before this virus hit, we were on shaky ground regarding our ability to weather a prolonged crisis like the COVID-19 pandemic. That is simply because most Americans have no savings to cover expenses if they lose their jobs. According to survey data from the U.S. Federal Reserve, 50% of U.S. households have no emergency savings, and 60% have no source of funds (including loans from family or friends) to cover three months of living expenses.[1]
More careful analysis of such data was recently conducted by health economist David Salkever, Professor Emeritus of University of Maryland, Baltimore County, and Johns Hopkins University. Dr. Salkever’s analysis of survey data from the Federal Reserve found that in October 2019, 42% of Americans said they felt at least one of the following signs of financial stress applied to them:
- They could not pay all their monthly bills.
- They could not cover $400 in emergency expenses.
- They were “just getting by” financially or worse.
In April of this year, as the COVID-19 crisis was intensifying, those reporting at least one of these signs of financial insecurity rose to 68% of the population.
Not surprisingly, use of health care services is inhibited by financial insecurity, and Dr. Salkever observed such effects in the Federal Reserve data. In October 2019, well before the COVID-19 pandemic began, absence of any of the three signs of financial stress corresponded to a 6% rate of missed medical visits, one sign to a 20% rate, and all three signs to a 46% rate. Moreover, these three simple indicators of financial hardship predicted missed medical visits in subgroups of those with low (less than $40,000), moderate ($40,000-$75,000) or high (greater than $75,000) annual household income (see graph).
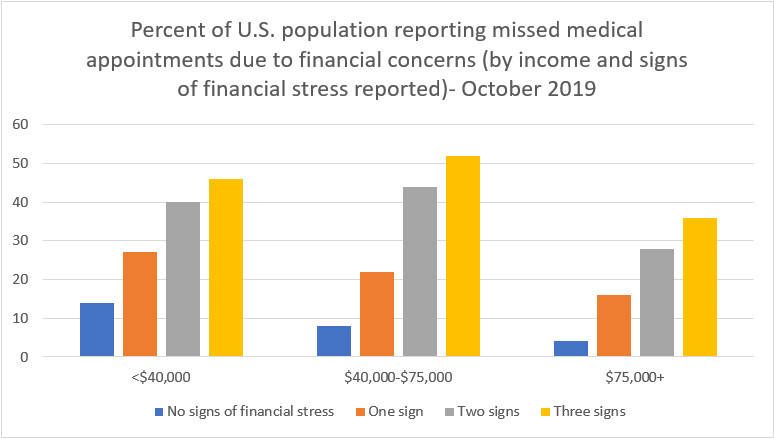
In its April 2020 survey, the Federal Reserve asked respondents what they would do if they got coronavirus symptoms. One-third of those who reported all three signs of financial stress said they would not seek medical attention. Such reluctance to obtain needed care is of grave concern because it suppresses two important responses to an infectious disease outbreak: early treatment, which may reduce individual illness progression, and early contact tracing, which is essential for dampening community spread.
And then there is the issue of race. People of color are disproportionately sickened and killed by COVID-19. Available death data spanning 45 states in the U.S. show that although Black Americans make up only about 13% of the U.S. population, they represent approximately 34% of those who have died from the virus so far. Economic challenges especially prevalent in Black populations appear to explain a substantial proportion of this outcome disparity. Black Americans, compared with white Americans, have lower incomes, lower rates of health insurance and higher rates of complicating conditions such as diabetes and obesity — all factors that increase the risk of bad health outcomes. However, statistical analyses that isolate the impact of race find that COVID-19 racial disparities persist even when the effects of income, insurance and other diseases are removed.
Accordingly, other negative correlates to racial inequity are implied. For example, Black Americans are more likely than white Americans to work in low-paying, frontline service or manufacturing sectors, placing them at especially high risk of infection. “People are having to decide between economic security and health security,” said Valerie Wilson of the Economic Policy Institute.[2] Obviously this is not a reassuring message for persons of color. Add to that the law enforcement actions that killed George Floyd, Freddie Gray, Eric Garner, Breonna Taylor and too many others, and it is not hard to see why folks are compelled to demonstrate loudly and persistently. Economic hardship and deadly pandemics are distinctive social stressors that demand thoughtful government-based responses.
Some reasonable solutions to lessen these inequities include passage of Medicare for All; guarantees of safe working conditions with protective measures and proper compensation if such measures are neglected or fail (for example, sick time or legal recourse); public infrastructure projects as economic stimulators (for example, roads, bridges, airports, schools and solar panels); policing reforms that demilitarize and desegregate law enforcement at every level of governance; sensible tax policies that redistribute wealth without erasing our deep desire for meritocracy; education, housing and criminal justice strategies that directly reduce and redress discrimination; and a social security system that creates savings funds to help us better adjust to future crises that greatly disrupt our economy. Let’s get to work on these things. Our way of life as a civil, democratic, productive society depends upon it.
References
[1] Harrison D. Lack of savings worsens the pain of coronavirus downturn. The Wall Street Journal. April 15, 2020.
[2] Vanek Smith S, Rosalsky G. Black Americans bear the brunt of the COVID-19 pandemic’s economic impact. Morning Edition, National Public Radio. June 3, 2020. Transcript.